 Open Access
Open Access
REVIEW
Investigating the Mental Health of Left-Behind Children in China’s Rural Areas: A Systematic Review Approach
1 Institution of International and Comparative Education, Beijing Normal University, Beijing, China
2 Department of Human Development, Teachers College, Columbia University, New York, NY, USA
3 Faculty of Education, Beijing Normal University, Beijing, China
* Corresponding Authors: Jian Li. Email: ; Eryong Xue. Email:
(This article belongs to the Special Issue: Child and Adolescent Mental Health: Risk and Protective Factors, Assessment, Interventions and Lifespan Outcomes)
International Journal of Mental Health Promotion 2026, 28(3), 1 https://doi.org/10.32604/ijmhp.2026.073286
Received 15 September 2025; Accepted 30 December 2025; Issue published 31 March 2026
Abstract
Background: The mobility of people in rural areas may lead to more and more left-behind children (LBC) appearing, and being an LBC brings a lot of risks to mental health, which could greatly hinder children’s development and undermine their happiness and safety in life. Previous scholars have conducted plenty of studies that focused on Chinese rural LBCs’ mental health issues, such as what they exactly look like and some potential factors, but there remains a paucity of reviews about the relationship among certain mental health issues. We will try to figure out how the most common mental health issues of LBC in China’s rural areas correlate with each other, as well as their related factors. Methods: In this study, we used a systematic review approach to analyze 35 publications from Web of Science and EBSCO (to August 2025), followed by the sorting standards of Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2020. Results: By mainly using quantitative techniques, we found that Chinese rural LBC are more likely to have mental health issues than children who have no experience of being left behind, and they often suffer from depression, social anxiety, internet addiction, and suicidal ideation. These four mental health issues share influencing factors and positively correlate with each other. We also found that Chinese rural LBCs are somewhat resilient towards the risk factors of mental health issues, and national or social policies and interventions can really help them a lot. Conclusion: For Chinese rural LBC, there are important relationships among the common psychological disorders they often suffer, along with multiple factors that affect their mental health, which can help related scholars and practitioners pay attention to such mechanisms and think more comprehensively when they try to help the children who are left behind.Keywords
Supplementary Material
Supplementary Material FileChildren who remain in their hometowns while their parents migrate to other regions for work are commonly referred to as “left-behind children” (LBC). These hometowns may be either rural or urban, though most are rural. China’s rapid economic growth and urbanization have created many employment opportunities in cities, prompting large numbers of rural residents to migrate for work. Because of the high cost of living in cities and limited access to healthcare and education, these adults usually do not bring their children with them [1]. This phenomenon is particularly evident in rural China. As urban living expenses and educational costs are higher, many migrant workers leave their children in their hometowns, entrusting their care to grandparents or other relatives [2]. Consequently, a large and distinct group of “rural LBC” has emerged [2]. According to China’s 2000, 2010, and 2020 censuses, the number of LBC in China was 30.09 million in 2000, 54.91 million in 2010, and 66.93 million in 2020 [3]. In these three censuses, rural LBC accounted for 26.99 million, 39.7 million, and 41.7 million, respectively, representing the majority of all LBC nationwide [3]. In this study, LBC are defined as children under the age of 18 who live in rural areas where one or both parents have migrated for work and cannot reunite with them for more than six months each year [4].
The physical and mental health of LBC is exposed to greater and more diverse risks compared with children living with both parents, and they are more likely to generate psychological problems in such living conditions. Rural LBCs usually have impaired self-awareness, dysfunctional relationship with their parents, and usually live in an imbalanced social environment [5]. Such conditions can contribute to strong negative effects on the mental health and behavior of rural LBCs, and very likely to make problems like social anxiety or internet addiction appeared. Social anxiety is a very unique and prominent type of anxiety in LBC, and the definition of social anxiety in this study is the noticeable concern or uneasiness brought on by the possibility or existence of one’s own assessment in actual or hypothetical social settings [6,7,8]. These risks have made the mental health of LBC an important social concern in contemporary China [5]. Besides, the risky factors like negative life events, the things that happen during a normal lifetime that can bring negative impacts or harmful effects on an individual’s physical or mental health [9]. Regardless of whether they live in rural or urban areas, prolonged separation from parents has been shown to cause significant psychological harm and even elevate the risk of substance abuse among LBC [10].
Another fact is that the factors from rural LBCs themselves can bring very huge impacts, which sometimes can really help rural LBCs deal with the risky factors in their lives. For example, their self-concept, a multidimensional mental concept that defines people’s mental representation of how well they are accepted by society and other people, how they consider their academic and athletic prowess, behavior, and physical expressions [11], or their psychological capital, an individual’s positive psychological state of development that usually has characteristics like having confidence (efficacy) to take on and put in the necessary effort to succeed at challenging tasks or persevering toward goals and, when necessary, redirecting paths to goals (hope) in order to succeed [12], or subjective well-being, a comprehensive index that incorporates both reflective subjective judgments of life satisfaction and emotional responses to ongoing life in terms of positive and pleasant emotions versus unpleasant and negative feelings [13]. Even though these factors are mainly affected by rural LBCs, some of these factors, like social capital, the social ties between the adults and kids who live there [14,15], are very likely to be affected by the environments. We will specifically discuss how these factors influence the mental health of rural LBCs.
While previous studies have explored common mental disorders and abnormal psychological states among LBC and examined a range of contributing factors, few have systematically linked these disorders to their associated determinants. Moreover, a comprehensive understanding of the mechanisms through which these factors lead to the psychological problems commonly experienced by LBC remains lacking. Although some studies have examined relationships between specific mental health issues among rural LBC, they typically focused on only one or two problem types, offering limited comprehensiveness. Therefore, this study aims to summarize the major mental health problems faced by rural LBC in China, clarify the interconnections among these problems, and analyze existing intervention strategies addressing their psychological well-being. The research questions (RQs) of this study are as follows:
RQ1: What are the main manifestations of mental health issues among Chinese rural LBC? What are their main characteristics?
RQ2: What are the personal, socioenvironmental, and macro factors of mental health of Chinese rural LBC?
RQ3: Are there any connections between the most common psychological problems among Chinese rural LBC?
RQ4: What are the current interventions or policies related to Chinese rural LBC’s mental health? How effective are they?
The reporting of this review adheres to the PRISMA 2020 guideline [16], and the completed PRISMA checklist is provided as Supplementary Material S1. This study employed a systematic analytical approach to examine existing research on the mental health of Chinese left-behind children, in accordance with the PRISMA 2020 framework. The databases used for literature retrieval were EBSCO and Web of Science. Before August 2025, 609 and 83 studies were retrieved from Web of Science and EBSCO, respectively, using the search terms “left-behind children” AND “mental health”. We also used some MeSH terms in our search, such as “COVID-19”, “Internet addiction”, and “Depression”. The retrieved literature was then limited to peer-reviewed, full-text journal articles written in English and published in core databases. After removing duplicates, 330 studies remained.
During the screening process, titles, abstracts, and keywords were checked against predefined exclusion criteria, resulting in the removal of 175 studies and the retention of 155. A further eligibility assessment of the full texts led to the exclusion of 119 additional papers (See Fig. 1).
This review adhered to the PRISMA 2020 guideline; however, it was not registered in PROSPERO, as registration is not mandatory for non-clinical or educational systematic reviews. The PRISMA checklist is provided as Supplementary Material to ensure reporting transparency (Table 1).
Table 1: Literature exclusion criteria.
| Order | Exclusion Criteria |
|---|---|
| Code 1 | Meta-analysis |
| Code 2 | Not on left-behind (left-behind elders, adults, college students, etc.) |
| Code 3 | Not on children in China (Romania, Philippines, Sri Lanka, etc.) |
| Code 4 | Not on mental health (behavioral problems, physical health) |
| Code 5 | Focuses on overseas or international left-behind children and urban left-behind children |
| Code 6 | Not SSCI |
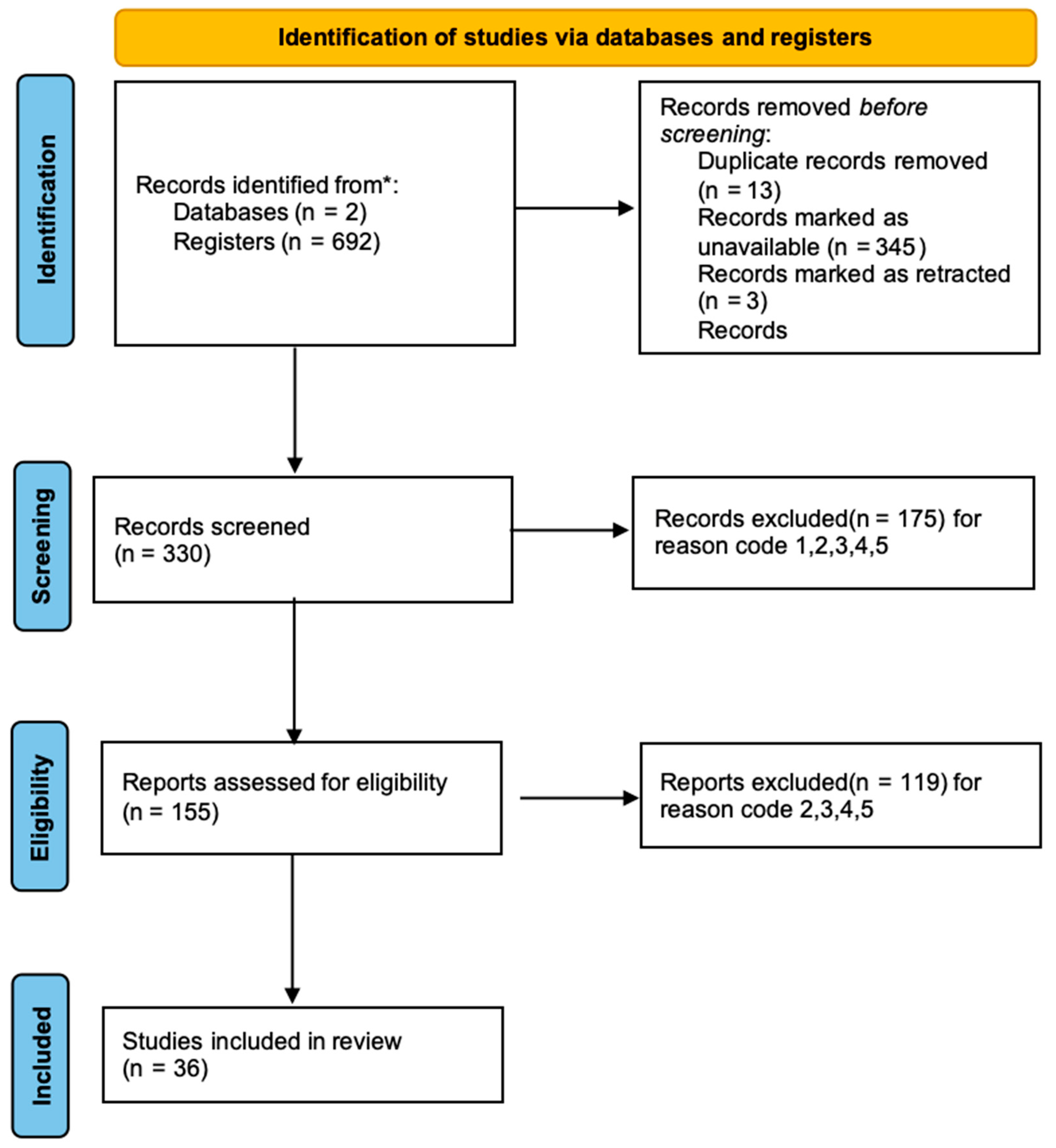
Figure 1: The publication screening process.
As shown in Fig. 2, the included studies covered most provinces of China; however, the number of studies conducted in Northwest China was notably limited. This pattern reflects a genuine lack of published research rather than an omission in our inclusion process. During the systematic search, only a few empirical studies focusing on the mental health of left-behind children were found in this region. This scarcity may be attributed to the uneven distribution of research resources, difficulties in data collection in sparsely populated rural areas, and the concentration of research institutions in eastern and central China.
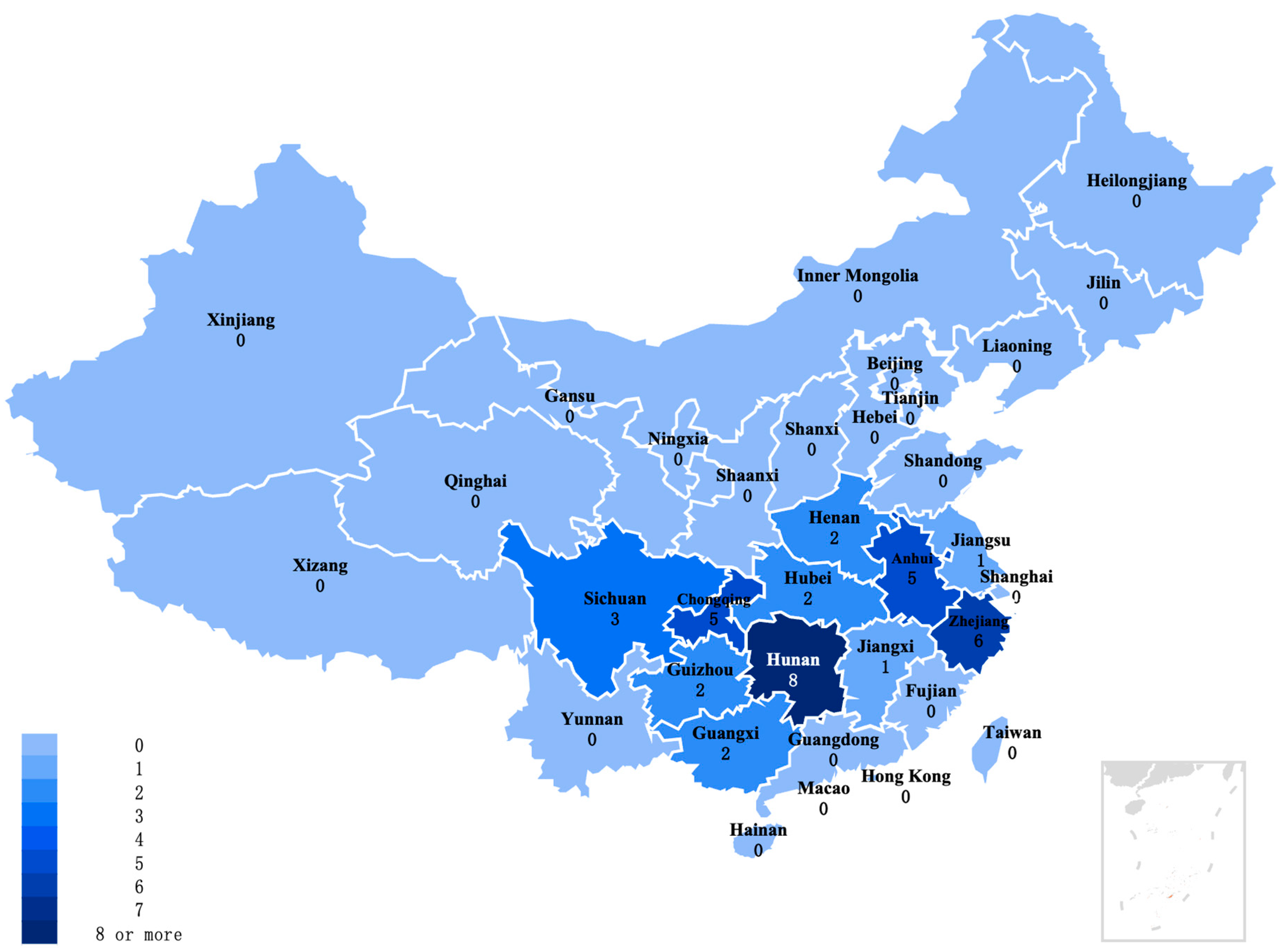
Figure 2: Distribution of study settings in the studies included in this study.
The screening, data extraction, and quality appraisal were conducted independently by two reviewers to ensure methodological rigor and reduce bias. Both reviewers first screened the titles and abstracts of all retrieved records, followed by full-text assessments of potentially eligible studies based on predefined inclusion and exclusion criteria. Any disagreements in study selection or data extraction were discussed and resolved through consensus.
For the quality assessment, appropriate tools were used depending on study design: the Critical Appraisal Skills Programme (CASP) [17] checklist for qualitative studies, the Joanna Briggs Institute (JBI) [18] checklist for quantitative studies, the Mixed Methods Appraisal Tool (MMAT) [19] for mixed-methods studies. Each study was scored according to the respective criteria, with higher scores indicating better methodological quality. The quality ratings are presented in the summary table (Table 2) alongside each study’s appraisal results.
To evaluate the consistency of the assessment process, inter-rater reliability was calculated using Cohen’s kappa, with values ranging from 0.875 to 1.000, indicating excellent agreement between the two reviewers in study selection and quality assessment.
Table 2: Summary of the included studies and quality appraisal results.
| Studies | Research Theme | Methodology | Main Findings | Sample Size | Study Design | Score (Risk) | Cohen’s Kappa |
|---|---|---|---|---|---|---|---|
| Wang et al. (2015) [20] | Depression prevalence | Quantitative | High depression rate: frequent parent–child communication is protective | n = 4857 | JBI | 10 (Low) | 1 |
| Zhang et al. (2023) [21] | Depression trajectory & parental support | Quantitative | Parental support lowers the initial depression level | n = 286 LBC + 129 NLBC | JBI | 10 (Low) | 1 |
| Shen et al. (2015) [22] | Parental migration & mental health | Quantitative | Academic performance and social support predict depression/anxiety | n = 2283 | JBI | 10 (Low) | 1 |
| He et al. (2012) [23] | Depression risk & social support | Quantitative | Low social support greatly increases depression risk | n = 875 (590 LBC) | JBI | 10 (Low) | 1 |
| Yang et al. (2021) [24] | Maltreatment, food security & depression literacy | Quantitative | Food security and depression literacy jointly moderate maltreatment–depression link | n = 1469 | JBI | 10 (Low) | 1 |
| Ho et al. (2018) [25] | Depression literacy & help-seeking attitudes | Mixed study | Higher depression knowledge is linked to more positive attitudes and a greater help-seeking tendency | n = 455 (survey) + 56 (focus groups) | MMAT | 10 (Low) | 1 |
| Bao et al. (2025) [26] | Internet gaming disorder (IGD) | Qualitative | Gaming addiction, shaped by family and cultural context negatively affected mental health, academic performance, and parent–child relationships. | n = 35 (21 students, 7 parents, 7 teachers) | CASP | 9.375 (Low) | 0.875 |
| Miao et al. (2024) [27] | Internet addiction, anxiety & suicidal ideation among left-behind children | Quantitative | Anxiety mediates, and social support moderates the link between Internet addiction and suicidal ideation; the effects are strongest for mother-only migrant families | n = 2882 (middle school students, age 12–17) | JBI | 10 (Low) | 1 |
| Fan et al. (2023) [28] | Revision and validation of an Adversity Scale for Left-behind Children (LBC) in rural China (updating the 2011 version based on the 2016 LBC definition). | Mixed study | Revised scale (33 items, 8 factors) showed a good model fit and reliability, demonstrated expected validity correlations, and LBC reported higher adversity than non-LBC | Valid N = 4428 total; LBC n = 2541 (also included formerly LBC n = 462; non-LBC n = 1425). | MMAT | 10 (Low) | 1 |
| Zhang et al. (2024) [29] | Social anxiety profiles, online communication & social capital among left-behind children | Quantitative | Latent profile analysis identified three anxiety types; higher online communication and social capital linked to greater social anxiety | n = 1358 LBC (junior middle school students, aged 12–16) | JBI | 10 (Low) | 1 |
| Xiao et al. (2019) [30] | Suicide ideation and suicide plan among Chinese left-behind children | Quantitative | One-week SI = 6.76%, lifetime SI = 20.8%; girls, self-harmers, and depressed children more likely to have SI; resilience—especially emotion regulation—protects against SI; depression is the key risk for transition from SI to suicide plan | n = 2898 (aged 10–18, Guangnan County, Yunnan) | JBI | 10 (Low) | 1 |
| Fu et al. (2017) [31] | Parental absence, emotional disorders & suicide ideation | Quantitative | Both-parents absence ↑ suicide ideation, depression, social anxiety, and physical anxiety mediate this link | n = 4513 (1997 LBC; ages 9–17, Yancheng, China) | JBI | 10 (Low) | 1 |
| Liu et al. (2021) [32] | Age at parental separation and mental health symptoms | Quantitative | Earlier separation age strongly predicted higher anxiety and depression; Guizhou children showed more symptoms than Anhui peers | n = 592 LBC (rural Guizhou and Anhui; ages 8–17) | JBI | 10 (Low) | 1 |
| Liu et al. (2010) [33] | Parental absence, self-concept & loneliness | Quantitative | LBC had lower self-concept and higher loneliness; parental/guardian relationship and activity time predicted self-concept | n = 216 LBC + 240 non-LBC | JBI | 10 (Low) | 1 |
| Ye et al. (2020) [34] | Subjective well-being & parent–child communication among left-behind children | Quantitative | LBC showed lower family and environment satisfaction; frequent parent–child contact increased positive affect and life satisfaction | n = 1086 (365 LBC; ages 12–18, Zhejiang Province) | JBI | 10 (Low) | 1 |
| Ren et al. (2021) [35] | Psychological capital & mental health of left-behind rural children | Quantitative | Higher psychological capital predicted better mental health; gender, age, and residence had no significant effects | n = 332 LBC (Grades 4–6, Xiangtan, Hunan) | JBI | 10 (Low) | 1 |
| Liu et al., 2009 [36] | Age at parental separation & anxiety/depression | Quantitative | Younger separation age predicted higher depression and anxiety; effects strongest for mother or both-parents absence | n = 592 LBC (ages 10–17, Anhui, Chongqing, Guizhou) | JBI | 10 (Low) | 1 |
| Liang et al. (2022) [37] | Eating habits and mental health among left-behind children | Quantitative | Unhealthy eating patterns (skipping breakfast, low fruit intake) depression, anxiety, and insomnia; associations stronger in females | n = 3314 LBC (aged 12–17, Guangxi Province) | JBI | 10 (Low) | 1 |
| Wang et al. (2022) [38] | Parental migration & adolescent mental health symptoms | Quantitative | Left-behind children showed higher depression; bullying, loneliness, and stress increased symptoms; social support reduced risk | n = 1347 (7th graders, 36.5% LBC) | JBI | 10 (Low) | 1 |
| Qi and Wu (2024) [39] | Parenting styles and rural children’s mental health: mediating role of mental resilience | Quantitative | Parental and intergenerational parenting affect mental health; mother–child relationship strongest; resilience mediates parenting effects | CEPS 2014–2015 dataset (approx. 20,000 students, rural subset analyzed) | JBI | 10 (Low) | 1 |
| Wu et al. (2014) [40] | Social capital and mental health among rural children with parental migration experiences | Quantitative | Left-behind children had higher depression; family and community social capital mediated migration effects; girls and boarding students reported lower social capital and higher depression | n = 701 | JBI | 10 (Low) | 1 |
| Han and Xu (2022) [41] | Negative life events, resilience, and peer attachment in left-behind children | Quantitative | Both-parents absent children had poorer mental health and lower resilience; resilience mediated effects of negative life events; peer communication improved resilience, while alienation worsened outcomes | n = 1030 | JBI | 10 (Low) | 1 |
| Xie et al. (2022) [42] | Parent–child attachment, peer relationships, and mental health of left-behind children | Quantitative | Secure attachment and positive peer relationships improved mental health; peer relations partially mediated the attachment–mental health link | n = 928 | JBI | 10 (Low) | 1 |
| Gao et al. (2023) [43] | Bullying, hopelessness, and grit | Quantitative | Bullying increased depression; hopelessness mediated; grit buffered effects | n = 476 | JBI | 10 (Low) | 1 |
| Wu (2023) [44] | Mental health of left-behind children before and after COVID-19 | Quantitative | Mental health improved after the pandemic; higher self-esteem and social support promoted well-being | n = 82 | JBI | 10 (Low) | 1 |
| Hou et al. (2021) [45] | Suicidality and its associated factors among left-behind and non-left-behind children during the COVID-19 pandemic in rural China. | Quantitative | Anxiety and depression predicted suicidality; coping style differed by LBC status | n = 761 (468 LBC, 293 NLBC) | JBI | 10 (Low) | 1 |
| Zhang and Yang (2019) [46] | Food insecurity, depression, and school performance among left-behind children | Quantitative | Food insecurity predicted poorer school performance; depression and educational expectation fully mediated this link | n = 2128 | JBI | 10 (Low) | 1 |
| Fu and Zhou (2022) [47] | Suicidal ideation and related factors among left-behind children | Quantitative | Suicidal ideation higher in left-behind children; depression and family conflict were main predictors | n = 1333 | JBI | 10 (Low) | 1 |
| Zhao et al. (2020) [48] | Resilience, self-esteem, and depression | Quantitative | Trait resilience mediated the link between social support and self-esteem and depression in left-behind children | n = 345 | JBI | 10 (Low) | 1 |
| Guo et al. (2015) [49] | Resilience and influencing factors | Quantitative | Higher resilience is linked to better mental health and fewer conflicts | n = 1403 | JBI | 9.375 (Low) | 0.875 |
| Fan and Lu (2019) [50] | Perceived social support, resilience, and mental well-being of left-behind children | Quantitative | Perceived social support directly improved mental well-being, with resilience playing a partial mediating role | n = 476 | JBI | 10 (Low) | 1 |
| Man et al. (2017) [51] | Development and function of China’s child protection system | Qualitative | The pilot system serves vulnerable children but lacks clear agency roles and effective reporting; a framework has been established, but faces cultural and structural barriers | n = 97 documents + 11 interviews | CASP | 9.375 (Low) | 0.875 |
| Sun et al. (2022) [52] | Mental health training of primary care physicians in rural China | Quantitative | Training significantly improved PCPs’ confidence and mental health care practices | n = 673 | JBI | 10 (Low) | 1 |
| Wang et al. (2022) [53] | Social support and positive psychology intervention | Quantitative | Intervention improved well-being and reduced depression | n = 70 | JBI | 10 (Low) | 1 |
| Ren and Li (2020) [54] | Physical exercise & social anxiety | Quantitative | Social support mediates and moderates the link between exercise and anxiety | n = 797 | JBI | 9.375 (Low) | 0.875 |
| Shang et al. (2023) [55] | Internet addiction and mental health among left-behind adolescents | Quantitative | Internet addiction increased later depression and anxiety; resilience and friendship quality mediated this relationship | n = 1001 | JBI | 10 (Low | 1 |
3.1 LBC’s Mental Health Issues Are Mainly Reflected in Some Specific Mental Illnesses or Abnormal Mental States
When previous researchers talked about LBC’s mental health, their research mainly discussed the very common mental illnesses or abnormal psychological states among left-behind children.
3.1.1 The Depression among Chinese Rural LBC
The first thing we need to discuss is depression, one of the most common mental illnesses among Chinese rural LBC. Its situation on LBC is different from an ordinary situation. In a study about how the LBC and LBAs (left-behind adolescents)’ depressive symptoms look like, the researchers selected 4857 participants from 7 to 17 years old whose parents are working outside Chongqing and leave them in Chongqing and found that 24.8% of those surveyed LBC and LBA have depressive symptoms, which is a huge proportion [20]. When doing a longitudinal study of the developmental trajectory of depression in LBC, compared to non-left-behind children (NLBC), LBC not only have more serious initial statuses of depression, but also show a clear upward trend later in life [21]. Moreover, the individual differences in initial levels and developmental trajectories are more pronounced than for NLBC [21].
LBC’s depression can be affected by many factors. Shen et al. designed a study to uncover how different parental migration patterns (no parents went out for work, father went out for work, mother went out for work, or both parents went out for work) correlates to the risk that Chinese rural children would suffer from depression or anxiety disorder by selected 2283 middle school students aged 10–18 years in Nanle County of Henan province [22]. The proportion of LBC in the sample is 61.2%, and LBC whose both parents went out for work have the highest rate of depression (14.2%), while there are 11.7% of the children whose father or mother went out for work suffer from depression [22]. By using Child Depression Inventory (CDI) to evaluate the risks of suffering from depression among LBC and compare them with the control groups (Children from rural areas, never been left-behind before, their parents were accompanying with them), He et al. got the results that shows that the risk of developing depression among LBC are greater than children have no experience of being left-behind [23].
Meanwhile, among LBC, there are greater risks of suffering from depression for children whose families are at low socioeconomic status (SES) than those families at middle or high SES, and children with low social support have a higher probability of suffering from depression than LBC children have moderate and high social support [24]. A study surveyed 1469 adolescents aged 12 to 18 years in junior high school from rural Hunan Province and used a hierarchical moderated regression model to find that maltreatment and food insecurity both have a strong positive correlation with depression among LBAs [24]. Besides, depression literacy, the capacity to identify depression and make informed choices regarding its treatment [25], also has an impact on LBAs’ depression, in which when the level of food insecurity and depression literacy are both high or both low, the relationship between maltreatment and LBAs’ depression will be significantly stronger [24].
3.1.2 The Internet Addiction among Chinese Rural LBC
Another mental health issue that previous researchers have always talked about is internet addiction. It usually represents internet gaming disorder or social media addiction. Many Chinese LBC are suffering from internet addiction. According to the February 2023 report “Investigation and Countermeasures on Mobile Phone Addiction of Left-behind Children in Rural Areas” published by Wuhan University’s Research Center for Chinese Rural Governance, Internet gaming has emerged as the primary activity for LBC in rural China [26]. Among them, the Internet gaming problem affects 5.66% of young LBC in Chinese rural areas, and 21.3% of parents believe that their kids have a severe addiction to online gaming [26]. Compared to children who are not experiencing or have experienced being left behind, LBC have a higher risk of becoming addicted to video games or social networking sites (SNS). By doing interview for 21 left-behind children about things like the impact of playing video games, seven parents about their attitudes towards children playing video games, and seven teachers about how they intervene in their students’ gaming behaviors, Bao et al. got the conclusion that the risks of LBC in rural areas suffer from internet gaming disorder may be attributed to the situations like there are no enough cultural infrastructure in rural areas or LBC’s parents and peers don’t give them correct guidance [26]. In order to figure out the specific situation of internet addiction among LBC in rural areas, the suicidal ideation of LBC, as well as some related factors, Miao et al. designed a cross-sectional study that mainly used a survey and invited 2882 left-behind children from 12 to 17 in rural areas of Chongqing [27].
3.1.3 The Social Anxiety and Suicidal Ideation among Chinese Rural LBC
Social anxiety is another mental health issue that is common among LBC in Chinese rural areas, and we will discuss it with another common mental health issue, suicidal ideation. Because Chinese rural LBC are highly likely to experience more risky factors of social anxiety, the social anxiety among Chinese rural LBC is much more serious than that of NLBC. These risk factors include perceived discrimination, poor learning management, poor communication, less accessibility to welfare, less parental guidance, a desolate home environment, less attention from their parents, and a lack of family resilience [28]. According to a latent profile analysis of social anxiety among Chinese LBC and LBA, among 1358 LBC and LBA from southwest China who participated in the study, social anxiety was higher among girls than among boys, higher among high school participants than among primary school pupils, higher among LBC whose parents were migrants than among other LBC, and lower among LBC who lived in an intact household [29].
For suicidal ideation, it is often discussed by scholars as a manifestation of mental illnesses such as depression or internet addiction, which are very common among LBC in Chinese rural areas. It always co-occurs with suicidal plans. Xiao et al. studied the prevalence and associated factors of suicidal ideation and suicidal plan in Chinese LBC by conducting a survey-based study of 2898 LBC who had not reached 18 years old in Guangnan county [30]. They found that the proportions of people who had suicidal ideation in the past week and had suicidal ideation in their lifetime were 6.76% and 20.8%, respectively, while the proportion of people who had a suicidal plan was 2.31% and 7.69% respectively, and such prevalence rates of suicidal ideation and suicidal plan are much higher among girls than boys [30]. Suicidal ideation usually leads to LBC hurting themselves. This proportion is almost three times the proportion of LBC with suicidal ideation among LBC who did not engage in hurting themselves [30]. Fu et al. designed a study about the potential for parental absence to predict Chinese rural LBC’s suicidal ideation, and they selected 4264 children from rural areas in Yancheng, China, who consisted of 2324 NLBC and 1940 LBC from 9 to 17 years old [31]. According to their results, 255 NLBC had suicidal ideation, and a total of 254 left-behind children had suicidal ideation [31]. At the same time, among groups of different types of parental absence, the prevalence rate of suicidal ideation among LBC whose father worked away from home is 11.7%, LBC whose mother worked away from home is 14%, and the LBC whose both parents worked away from home is 14.1% [31]. Suicidal ideation has different kinds, such as passive and active suicidal ideation. Passive suicidal ideation, like a desire to die, does not have an actual plan or thoughts to hurt oneself, while active suicidal ideation, like a desire to kill oneself, does have an actual plan or thoughts of suicide [32]. By doing a study on 371 rural LBA from Henan, Liu et al. gained the results that approximately 15.90% LBA were currently experiencing “pure” passive suicidal ideation and 17.79% LBA were currently experiencing active suicidal ideation [32]. They also did a follow-up multivariate logistic regression, which shows that rumination and grit were the only factors that continued to be important in predicting passive suicidal ideation among LBA without active ideation after controlling for factors like age, sex, and depressive symptoms [32].
3.1.4 The Mutual Influence between These Mental Health Issues of Chinese Rural LBC
In fact, there is a strong correlation between these mental health issues that has caused great harm to many LBC. After analyzing by Pearson correlations, the results show that internet addiction is a strong mediating factor of the relationship between anxiety and suicidal ideation, that the internet can increase the level of anxiety of LBC, which in turn increases the possibility that LBC would generate suicidal ideation [27]. This may be because the causes of some mental illnesses and the possible consequences are relatively similar. For example, suicidal ideation and behaviors are possible consequences of depression. For LBC, if the environment they live in has risky factors common to multiple mental illnesses, their risk of suffering from multiple mental illnesses at the same time will also be very high. After all, it is not uncommon to suffer from multiple mental illnesses at the same time.
3.2 The Factors That Affect LBC’s Mental Health Are Diverse and Multifaceted
3.2.1 The Factors from Left-Behind Children Themselves
There are many kinds of factors that are related to LBC’s mental health, and they belong to different perspectives. First, LBC’s own characteristics can affect their mental health significantly. For example, the self-concept. A study about how the absence of parents can potentially affect Chinese rural LBC’s self-concept and loneliness invited 230 “absent migrant parents’ children and 250 comparison children (the children who do not experienced) in the rural areas of Yuan’ an County, and their data shows that the children of “absent migrant parents” had a lower level of self-concept higher level of loneliness than the comparison children, and self-concept is negatively correlated with loneliness while loneliness is a very strong predictor of mental health issues [33].
Another factor of LBC itself is subjective well-being. Ye et al. used a cross-sectional design method to investigate the subjective well-being of Chinese rural LBC, and they invited a total of 1086 children (365 LBC) aged 12–18 years from junior and senior high schools in a rural county of Zhejiang Province [34]. They used life satisfaction (such as environment satisfaction, family satisfaction, camaraderie satisfaction) and happiness (positive and negative affect), the two main elements that make up subjective well-being, to measure the subjective well-being of the students in their sample, and according to their results, LBC have less environment satisfaction and family satisfaction than NLBC [34]. These factors related to subjective well-being will indirectly be correlated with the risks of mental health of LBC. Besides subjective well-being, psychological capital is also an important mental characteristic for people’s mental health, and some studies have proved that LBC’s psychological capital is closely related to their mental health. By asking 473 rural LBC from Grades 4 to 6 in Xiangtan to do the survey questionnaire about their psychological capital and psychological health status and using the Pearson correlation coefficient to analyze how much the overall psychological capital scale correlated to mental health from all dimensions, Ren et al. found that LBC’s psychological capital is significantly positively correlated to their mental health [35]. The questionnaire about psychological capital includes 5 dimensions: independence and perseverance, gratefulness and sensitivity, kindness and indulgence, hopefulness and vigor, and assurance and guts, and these are all closely positively correlated with mental health issues [35]. There is another significant manifestation of psychological factors that has an indirect but important effect on LBC’s mental health, which is psychological resilience [35].
From another perspective, it is also possible that some of LBC’s own living conditions or physiological characteristics can affect their mental health to some extent. One factor that researchers have studied a lot is age, and there is evidence that age can play a very important role in the relationship between parental absence and LBC’s psychological well-being. According to a study about whether when Chinese rural LBC started to separate from their parents can affect the degree of their depression or anxiety that used 592 LBC from 10 to 17 years old from Chongqing, Anhui, and Guizhou’s rural area, the symptoms of depression of children who separated from their parents before they reached three years old are more serious than children who separated from their parents between the ages of three to six, and the symptoms of children who separated from their parents at 7 years old or older, which is the time they started to go to school, are fewer than children who separated from their parents prior to the age of 17 [36]. The difference in the effects of separation age on LBC depression and anxiety symptoms was most evident when comparing LBC before and after the age of seven [36].
Not only age, but the daily routine of LBC can also affect their mental health significantly. Some studies prove that left-behind children’s eating habits can affect their mental health. Liang et al. designed a cross-sectional study to explore the impact of left-behind children’s eating habits on their mental health, and they selected 3332 grade 1 to grade 3 students (2907 from rural areas) from one of the poorest areas of Guangxi, Hechi city [37]. According to their results, for females, how frequently they eat fruits, vegetables, and protein is negatively correlated to the severity of insomnia, depression, and anxiety; for males, the frequency of eating fruits is negatively correlated to the severity of insomnia [37]. Even the frequency of eating breakfast is closely related to the severity of insomnia and depression in both sexes [37].
3.2.2 The Outside Family and Social Environments
When considering the outside, the family situation, and the living environment of LBC can bring significant impacts on their mental health. Even among LBC, the situation of the main family members working outside may also vary. Some may have their father working away from home, some may have their mother working away from home, and some may have both parents. These different parental migration situations can have different impacts on LBC’s mental health. There is a cross-sectional study that used data from an intervention-focused research which asked 1347 seventh-grade children (492 LBC) from four rural junior high schools in Northeastern Hunan Province shows that LBC with different types of parental absence (mother or father not at home, both parents not at home and both parents at home) will show noticeable differences in the incidence of depression symptoms [38]. Compared to LBC whose father works away from home or both parents work away from home, LBC whose mother works away from home were more likely to suffer from depression or have any suicidal ideation [38]. Moreover, LBC whose fathers work away from home were most likely to get generalized anxiety disorder [38]. LBC are not necessarily unable to be with their parents all the time. Therefore, during the time they are with their parents, the parenting style adopted by their parents could generate a certain effect on LBC’s mental health. Parenting attitudes and behaviors are two subcategories of parenting style, which is the sum of the concepts, actions, and feelings that parents teach their kids [39]. Parenting behaviors are the actual acts parents take to feed and educate their children, while parenting attitudes are the information, ideas, feelings, and behavioral tendencies parents hold when raising and educating their children [39]. Parents also teach their children social values and views while they are parenting them [39]. Qiu and Wu used approximately 20,000 students in 28 rural counties from the 2014–2015 China Education Panel Survey (CEPS) database to study how different parenting styles affect rural LBC’s mental health, and their results show that both parenting behaviors and attitudes are strongly correlated to rural LBC’s mental health [39]. Parents who completely supervise their children’s education will benefit their mental health, while those who strictly supervise social interactions and other life events of their children will make their mental health issues worse [39]. Moreover, in most households, mothers are the primary caregivers for children and typically take on a loving role in raising the family [39]. Most children communicate with their mothers more frequently and in-depth, and they receive more support and care from them, all of which helps to lessen the mental health issues like anxiety and depression among LBC [39].
Social capital is another kind of social factor that is related to LBC’s life and mental health, and it has different types, such as family or community social capital, means connections to different social objects. Wu et al. have conducted research to explore how social capital may affect the mental health of Chinese rural LBC with different parent migration types, using 624 4th to 9th grade students (58.2% left-behind, 16.5% previous left-behind, 25.3% never left-behind) from Guizhou’s rural areas [40]. According to their results, family social capital is strongly negatively correlated with LBC’s level of depression, which is also true for community social capital [40]. Additionally, regardless of the kinds of left-behind experiences these children are currently undergoing or have previously experienced, they have higher depression levels than children who have never been left behind [40]. Furthermore, social capital in the family and community played a mediating role in the relationship between various left-behind statuses and LBC’s mental health [40]. The status variables, such as experiencing migration to other areas, whether they have or have not, significantly correlated with poorer family social capital levels, which predicted more serious depression, aside from the fact that those with no prior migration experience were previously left behind [40].
Moreover, uncertain factors from society or nature are also likely to have an impact on LBC’s mental health. Some studies have shown that negative life events have a certain level of correlation with LBC’s mental health. According to a cross-sectional comparative study exploring the potential effects of negative life events on Chinese rural LBC’s mental health that let 1368 fourth to seventh grade from rural primary and secondary school in Sichuan to do the questionnaires, among the 1030 valid questionnaires, the specific circumstances of parents working away from home are negatively correlated with the negative life events their children may experience, which means that LBC will experience more negative life events than NLBC, and both-parents absent LBC would experience more negative life events than single-parent absent LBC [41]. In addition, negative life events are negatively correlated to resilience and the mental health of LBC [41].
School bullying or bullying victimization is a kind of negative life event that is closely related to LBC’s mental health. In order to explore the serial roles that parent-adolescent communication and school bullying victimization played on Chinese rural LBC’s mental health, Xie et al. selected 2737 children (1054 current LBC, 780 experienced left-behind in the past) from Kaihua County in Zhejiang Province and Nanling County in Anhui Province, the mountainous rural areas in these two provinces, to take the survey [42]. The results show that among the group of current left-behind children, the proportion of bullying victimization is 22.7%, which is the highest among all the groups [42]. Additionally, for current left-behind children, school bullying is a positive predictor of mental health issues [42]. A study exploring the potential relationship between bullying victimization and depression among Chinese LBAs invited 1072 middle school children (476 left-behind children) from two rural junior high schools in G County (an economically depressed rural area) of Jiangxi Province, which found that experiencing bullying and feeling hopeless both had positive effects on LBAs’ depressive symptoms [43].
The outbreak of COVID-19 has had a huge impact on education and the lives of citizens around the world, including in China. Some studies have shown that COVID-19 can have some effects on the mental health of Chinese rural LBC by exploring the difference between the mental health statuses of Chinese rural LBC before and after COVID-19. Wu investigated 82 grade 4 to 6 rural LBC living in Anhui and used surveys like Symptom Check List-90 (SCL-90) for assessing LBC’s mental health statuses [44]. The results show that the score of LBC in their sample on the mental health status surveys before and after COVID-19 are very different, like their scores on items related to depression or anxiety, which means that the emergence of COVID-19 has indeed brought about significant changes in rural LBC’s mental health [44]. In more detail, the LBC in the sample had higher scores on the mental health survey during the COVID-19 epidemic than after the epidemic, indicating that their mental health was worse during the COVID-19 epidemic [44]. It is also a choice for previous studies to investigate the situation of Chinese rural LBC’s mental health during the COVID-19 pandemic. After making a comparative study between the suicidality of 468 rural LBC and 293 rural NLBC in Anhui Province when the COVID-19 was still raging, Hou et al. found that LBC had higher possibility to generate suicidal ideation (rate: 37.8%) and attempts (rate: 11.3%) than NLBC (suicidal ideation: 34.1%, suicidal attempts: 8.9%), and it further suggests that during the COVID-19 pandemic, the odds of suicidal thoughts and attempts among Chinese children living in rural areas were highly concerning [45]. During COVID-19, factors like anxious emotion towards COVID-19, the economic threat posed by COVID-19’s impact on parents’ jobs, or maladaptive tactics (like blaming themselves or others, or contemplating), are all positively related to the suicidal thoughts and attempts of these children in rural areas, including LBC [45].
3.2.3 Macroeconomic Factors Related to the National or Social Level and Other Relevant Factors
Some macro-level factors related to policies, such as resource allocation in different regions, may indirectly become factors of Chinese rural LBC’s mental health. For example, Chinese rural LBC’s mental health may be affected by how much they can access safe food. Zhang and Yang used a cross-sectional method to explore how food insecurity connects with how well LBC perform at school and depression, and educational expectations’ serial mediation on the focal connection, and they invited 2128 grade 5 to 9 Chinese rural LBC to participate in the study [46]. According to their results, food insecurity had a substantial direct impact on depression and educational expectations, and it was significantly positively correlated with depression [46].
The policy during the COVID-19 pandemic is another potential factor that can affect the mental health of LBC. Wu suggested that it is possible that the elimination of the closed-stay policy contributed to the significant improvement in the mental health of children who were left behind after the pandemic, as evidenced by the fact that their SCL-90 scores were lower than the national average [44]. Not only this, once the closed-stay policy is lifted, traffic roads can be restored, which can provide a sense of security to children who are left behind [44]. Additionally, students will be under less stress when classes resume normally than when they were taught online during the pandemic because offline learning is simpler, helps them learn new things, and allows them to interact with teachers and classmates more, which fosters positive interpersonal relationships [44].
The different social supports, especially supports from family, teachers or schools, and peers, are always discussed by previous scholars. A study about how parental migration could bring impacts on the mental health of Chinese children selected 1892 school-aged rural children (1066 LBC) from Sichuan, and found that the social supports from family, teachers, and peers were negatively correlated to LBC’s depressive symptoms, and higher social supports from family, teachers, and peers predict better mental health status [47]. Kinship care is a specific kind of social support. If all LBC parents work away from home, kinship care can reduce LBC’s perception of family support, which can make the risk of developing depression higher and their mental health worse [47]. If only LBC’s mother works away from home, kinship care can increase LBC’s expectations of support from their peers, which can weaken the negative impact of parents working away from home [47].
3.3 LBC Still Have the Ability and Potential to Be Resilient in Dealing with Factors that Threaten Their Mental Health
LBC are not completely defenseless against risk factors for mental health issues, both within themselves and those around them. They possess a certain level of resilience, both psychologically and physically, to help them adjust to these risk factors. Zhao et al. selected 345 LBC aged 12 to 17 in Huoshan County to explore the potential effects that psychological resilience may have on Chinese rural LBC’s mental health, and they found that supportive behaviors or events that can protect LBC strongly correlated to LBC’s self-esteem and depression, while self-esteem is a very important factor of LBC’s psychological resilience [48]. The protections LBC can receive in their lives, like receiving help from teachers and peers, their peers and family members have high expectations of them, are positively correlated to LBC’s self-esteem and negatively correlated to depression [48]. Additionally, there is also a positive correlation between the psychological traits like self-reliance or ambition and self-esteem, while these psychological traits are negatively correlated to depression [48].
There is a cross-sectional study about the resilience of Chinese rural LBC and how it is correlated to their mental health investigated 1401 students from middle school (1049 LBC) in Yunyang County discovered that the resilience of children who are left behind might be impacted by things including grade, conflict with the guardian, and their concern about the fact that their parents are working outside, and resilience is strongly positively correlated to mental health [49]. In addition, resilience is also a moderating factor of several specific psychological problems, such as social anxiety and a tendency to be oversensitive [49].
On the other hand, even if left-behind children do not have relevant resilience at certain times, they can also stimulate their potential through certain external means or conditions to help them gain stronger and more resilience. To investigate how perceived social support could affect LBC’s mental well-being, Fan and Lu invited 476 grade 4–9 LBC (422 rural LBC) in grades 4–9 based on a ChuZhou District’s school-based project that included 6 schools [50]. According to their results, not only do both resilience and perceived social support have a positive effect on LBC’s mental well-being, but LBC’s resilience can also be better if they have higher perceived social support [50]. Additionally, LBC’s mental health is significantly impacted by how much social support they expect from their family and peers, or someone they consider important, which suggests that there is a higher probability for children who have a higher perception of social support to experience positive outcomes related to their mental health [50].
3.4 National and Social Policies, Resources in the Surrounding Environments, and Targeted Interventions Have Very Important Impacts on LBC’s Mental Health
Relevant policies of the country and society are very important for LBC because they can have a great impact on their living environment. These impacts can be very helpful for their mental health. Early on, the things included in a system to protect children, like excellent interventions, can reduce violence or social anxiety lastingly, and maximize the industrial productivity in the long run, academic achievement, educational attainment, and health of LBC [51]. To figure out how to deal with the serious problems the LBC are facing, it is essential for scholars and related practitioners to think about the importance of such a system, and the methods to construct and release it [51]. Current community service organizations sometimes recruited groups of volunteers, the so-called “loving mothers” or “loving families”, to accompany LBC when they were with their families to give them more love, safety, and care [51]. Moreover, in many areas, childcare training and mental health consulting are developed by social organizations, schools, and social welfare agencies [51]. These expanded services enhance the standard of care for children who are left behind, which benefits the long-term development of LBC’s mental health [51]. Policies regarding the construction of local medical facilities can also have some beneficial effects on LBC’s mental health. Sun et al. designed a cross-sectional study in Zhejiang Province’s rural areas and invited 673 primary care physicians to participate to explore how the training about managing depression that the primary care physicians received may affect the anxiety of Chinese rural LBC and left-behind elders [52]. Their results show that almost a quarter of primary care physicians said their patients always talk about their mental health issues, while almost half said their clients sometimes talk about their mental health issues, which means that many left-behind elders and children indeed care about their mental health [52]. Additionally, for primary care physicians, receiving some relevant training can make them more confident when they try to diagnose and manage their patients, and the more time they spend in training, the more likely they are to encounter patients with psychological problems [52]. The demand for mental health protection for all people in rural areas, including left-behind children, is still very high. Only by ensuring the training of mental health intervention treatment skills of medical staff in rural medical institutions through national and social policies can we have a sufficiently strong positive impact on the mental health of people in rural areas, including LBC.
Not only policies, but some interventions targeting the mental health of LBC, although they may not be as influential as national and social policies, can also have a very positive impact on protecting the mental health of LBC. To explore how interventions about social support and positive psychology can affect LBC’s depression and subjective well-being, Wang et al. designed a longitudinal study that invited 70 LBC from a township (rural area) in the central China whose scores on Self-Rating Scale for Depressive Disorder are 15 or higher (which means that they have significant symptoms of depression) [53]. They designed a group counseling activities and intervention for developing positive psychological characteristics, which mainly focuses on developing the positive mental quality like compassion or persistence, and they found through the study that although the level of subjective well-being and depression between the LBC who participated in the intervention and those who did not didn’t show significant difference when the intervention just began, after the intervention started one year and two years, the LBC who joined the intervention shew significantly better subjective well-being and less severe depression than those who did not participate [53]. Actually, the interventions that focus on improving the physical health of LBC are also beneficial for LBC’s mental health. A study asked 1606 primary school students and secondary school students (797 LBC) aged 9 to 15 from rural areas in Hunan province to participate in an investigation, and got the results that gymnastics can have a significant impact on rural LBC’s social anxiety [54]. More specifically, exercise intensity, exercise time, and the frequency of exercising are all significantly negatively correlated to social anxiety [54]. If the intervention can encourage left-behind children to do more exercise, it may be helpful to improve LBC’s mental health.
The development of urban areas always attracts a lot of attention from managers and government practitioners since it has more resources and opportunities and is better able to highlight the image of a country. Therefore, the flow of resources and policy bias can easily lead to urban-rural imbalance. Urban areas have more job opportunities, easier access to more and better resources, and living conditions may be better than in rural areas, which makes many rural adults (especially in early and middle adulthood) choose to seek opportunities in more developed urban areas. Since these young and middle-aged people may have their own children, and when they go to the city to develop, they may not take their children with them due to various reasons. Therefore, as they leave the countryside to develop in the city, their children become LBC. Mental health is crucial for a child’s development. If mental health is damaged and becomes abnormal, children’s lives and development will be at great risk, and such risks may even be fatal. Many studies now show that when parents leave their original living area to live and work elsewhere, it will have a great impact on their children’s mental health, and most of the impacts are negative [21,22]. It is imperative for both Chinese educators and authorities, like governments, to allocate sufficient attention to helping maintain rural LBC’s mental health.
Previous research on LBC’s mental health has focused mainly on the main manifestations of their mental health issues and some related intervention methods. According to the previous studies, when talking about the issue of left-behind children’s mental health, there are four topics that previous researchers discussed a lot: “interventions”, “emotional problems” (especially depression and loneliness), “deviant behaviors”, and “family child-rearing strategies” [2]. Specifically, interventions-related researches are mainly aimed at creating systematic and feasible intervention programs for left-behind children, or specific intervention methods or related factors such as “social support system”, “group psychological guidance”, and “protection factors”; researches about emotional problems mainly focus on specific emotion-related issues such as mental health, depression, negative emotions, loneliness, and related influencing factors such as social capital, positive events in daily life, mental elasticity, guardianship, and there are also many discussions on other issues such as mental resilience [2]. Chinese scholars used to have more viewpoints on issues related to LBC’s development, but recently they turned their attention to the factors that can protect LBC’s development, also enhancing LBC’s abilities to adapt to the risky factors after learning about “mental resilience” and other positive psychology theories [2]. In this review, we found that the main manifestation of psychological problems among Chinese rural LBC is that psychological problems usually manifest themselves in the form of specific mental illnesses or abnormal mental statuses. The psychological problems like depression, social anxiety, internet addiction, and suicidal ideation are very common among Chinese rural left-behind children. Based on this finding, further study shows that these psychological problems are usually affected by many factors, and these factors are sometimes correlated to each other. For the personal factors of left-behind children, it could be psychological capital, self-concept or subjective well-being, and so on [33,34,35]. For social factors related to their family and living environments, the factors could be social capital, negative life events, school bullying, and so on [40,41,42]. For the macro-factors, it could be national policies or intervention programs from the country or society, and so on [44,46]. We do not need to be too pessimistic or worried about the LBC’s mental health issues, because the LBC themselves have some resilience to mental health issues, and they also have many resources and means to help improve their resilience to cope with mental health issues. In addition to LBC being able to improve their resilience through their own experiences and the environment, national and societal policies can also have a positive impact. Furthermore, many intervention programs targeting the LBC’s mental health have emerged and attained some good achievements.
The signs of mental health issues are usually the appearance of related symptoms or signs of mental illness. This is why we judge whether people have mental health issues by whether they show certain specific characteristics in their daily lives. Although LBC is a group that is relatively special, the ways to measure their mental health are not much different from those of the public, because the only difference between them and the general public in mental health is that they may suffer from more risk factors. The Fig. 3 shows the complex mechanism of how factors from different aspects affect the mental health of Chinese LBC.
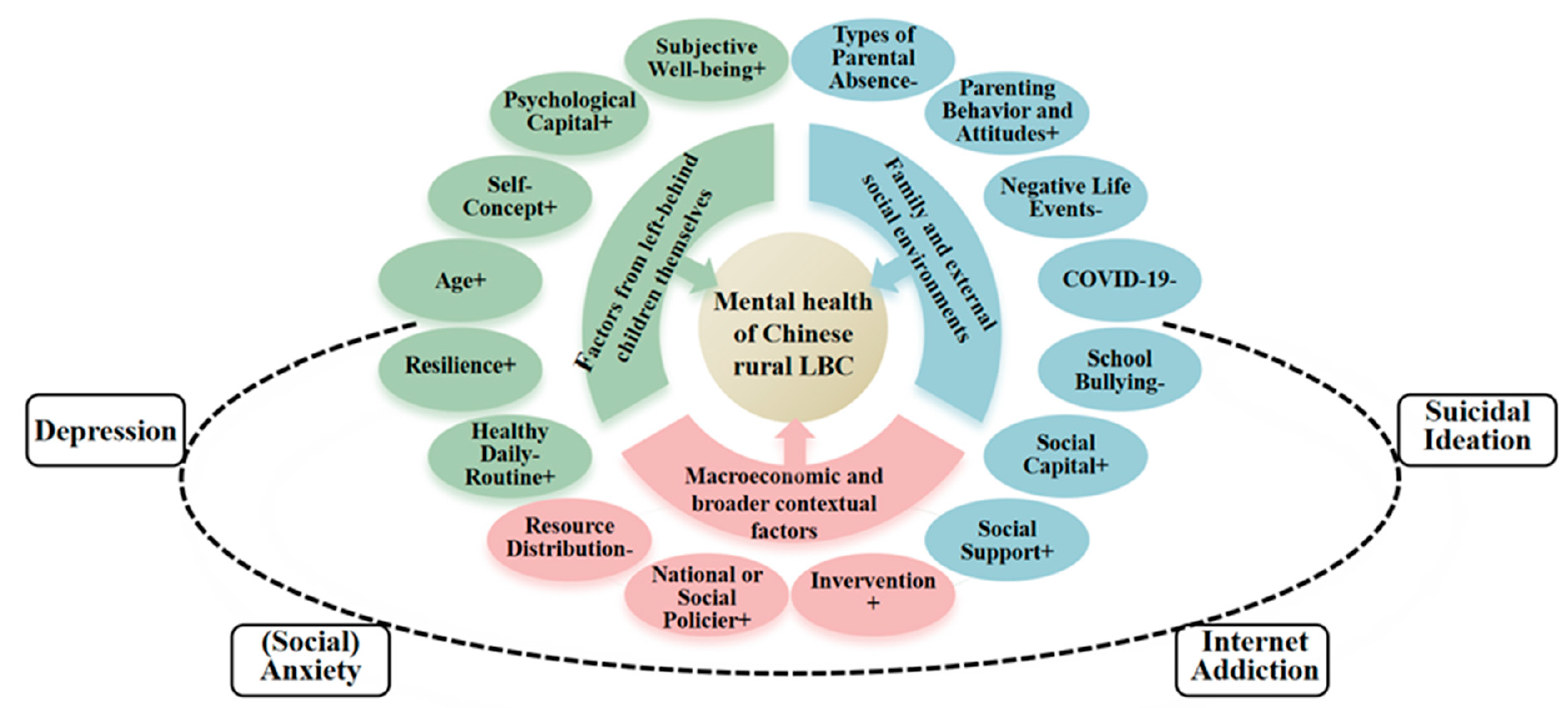
Figure 3: The characteristics of Chinese rural LBC’s mental health and its influencing factors.
In fact, there is a strong correlation between these mental health issues that has caused great harm to many LBC (see Fig. 3). Shang et al. drew data from a longitudinal study in two rural middle schools in China, and a total of 1001 LBAs aged 11 to 18 years were included. According to their results, among LBAs with depressive symptoms, 42.8% also had anxious symptoms, while among LBAS with anxious symptoms, 55.4% also had depressive symptoms, which shows a great co-morbidity [55]. Additionally, internet addiction is positively correlated to both depressive and anxious symptoms, suggesting that Internet addiction may increase the risk of LBAs developing depressive or anxious symptoms [55]. This may be because the causes of some mental illnesses and the possible consequences are relatively similar. For example, suicidal ideation and behaviors are possible consequences of depression. For LBC, if the environment they live in has risky factors common to multiple mental illnesses, their risk of suffering from multiple mental illnesses at the same time will also be very high. After all, it is not uncommon to suffer from multiple mental illnesses at the same time.
Exposure to bacteria, viruses, or other potentially pathogenic substances does not necessarily lead to illness, as the human body has an immune system. The same is true for mental illness: even if a person’s living environment presents risk factors for mental illness or experiences life events that have a significant impact on their psychological well-being, they may not necessarily develop a mental illness. This is because people possess psychological resilience, which helps them adjust after experiencing a traumatic event, a fact that also applies to left-behind children. Resilience is also influenced by many factors, both environmental and personal, which can have positive or negative impacts on resilience. According to Shang et al., internet addiction is positively correlated to both depressive and anxious symptoms, and friendship quality can generate a moderating effect on these two relationships [55]. At the same time, there is another positive correlation between friendship quality and LBC’s resilience [55]. Although rural LBC are indeed psychologically resilient, their resilience is usually weaker than NLBC’s resilience because their resilience is exposed to more risk factors and is therefore more easily weakened.
The issue of LBC has always attracted significant attention from the Chinese government and society. China has consistently worked to ensure the well-being, health, and education of LBC. Both the Chinese government and society have introduced numerous policies that can indeed help LBC. The successful implementation of these policies demonstrates that LBCs are not completely “left behind”, as the government and society continue to care for them. With the help of the country and the government, LBC can have more opportunities, and their living environment and conditions can be greatly improved, which can weaken the effects of risk factors related to mental health issues in their lives or even reduce those risk factors. The knowledge learned in school and the community may also help LBC improve their cognition, which is beneficial for their resilience.
The interventions to protect or provide care for LBC’s mental health are not necessarily formulated by the state and society. Although their radiation capacity may be relatively weak, they can really provide very powerful help in solving LBC’s mental health issues and their mental health development. Different LBC’s mental health issues may be significantly different in complexity and seriousness based on their general illnesses. Common illnesses like the common cold may be recovered from through non-medical measures or immune responses. However, mental health issues or illnesses are different. While people can use their own resilience to reduce the effects of risky factors, if they develop a full-blown mental health issue or illness, it is extremely difficult or impossible for them to recover by themselves. Therefore, external intervention is essential for the treatment of mental health issues. Effective intervention methods can significantly improve the speed and effectiveness of recovery from mental health issues. The intervention can provide LBC social support that can help them gain external resources and develop positive psychological qualities, so LBC will find it easier to procure internal resources and have stronger subjective well-being, which will reduce their risk of depression and improve their mental health [53]. When LBC has more opportunities and resources, it will be easier for them to rebuild their psychological defenses against mental health issues, allowing them to rid themselves of the negative effects of risk factors more quickly. For LBC, effective interventions may help them identify the root causes of their mental health issues and provide them with effective coping strategies. Intervention programs may also enrich their spiritual and daily lives while providing them with adequate care and a sense of security. These efforts can help left-behind children with mental health issues recover more quickly. For LBC who don’t currently have a confirmed mental health issue, participating in such interventions can also help them better avoid and address potential risk factors in their lives, ultimately protecting their mental health.
Other Asian countries, such as the Philippines, have certain similarities with China in the current situation and handling of the LBC issue. Due to the large-scale outsourcing of labor in the Philippines, the problem of LBC cannot be ignored. The Philippines is the fourth-largest recipient of remittances globally and one of the top exporters of labor [56]. Factors associated with mental health issues faced by Chinese rural LBC are like those faced by LBC in the Philippines. Among Filipino children, parental separation is most likely to be linked to feelings of sadness, worry, and loneliness [57]. Also, compared to NLBC, Filipino LBCs have a greater risk of having common mental health issues like depression or anxiety, which is like the situation in China [56]. Besides the situation, China and the Philippines also have many similarities in their interventions for LBC’s mental health issues. In the Philippines, the intervention programs for LBC’s mental health issues can be categorized into four levels, and all four levels can comprise a pyramid called the Inter-Agency Standing Committee (IASC) intervention pyramid [57]. The second level of this pyramid represents the largest proportion of interventions, which focus on strengthening community and family settings [56]. The programs at this level usually aim to utilize social networks to provide LBC peer support, educational activities, social events, and youth camps [58], and aim to provide educational services, such as training teachers to support students in schools [57]. China’s main interventions and support for rural LBC also include providing social resources for LBC and training relevant practitioners to support them. Therefore, the insights gained from this study on the mental health status of Chinese rural LBC and related intervention measures will not only benefit China but may also benefit other Asian countries with similar situations.
There are indeed some limitations in this study. First, this study only focuses on rural LBC. In fact, LBC are not only found in rural areas but also in urban areas. Some residents with children who live in less developed cities may move to more developed cities or even other countries to seek better development conditions and opportunities. In this way, their children will also become LBC. There have been some studies on the mental health of left-behind children in urban areas, and these studies have shown that the mental health of left-behind children in urban areas faces more challenges than that of NLBC. Because this study only focuses on the mental health of LBC in rural areas, it cannot represent the entire group of LBCS. Second, most of the studies selected for this systematic review were published relatively long ago. China has achieved very rapid and remarkable development in the past few decades, but as development continues, the problem of LBC has been constantly changing due to factors such as the continuous updating and improvement of policies and changes in resource allocation. If the research started too long ago, the various conditions and situations at the time of the research will be very different from those of today, so the results obtained may not be applicable to the current situation. This systematic review has relatively few studies on the LBC’s mental health in recent years, so it does not have enough novel research that can better reflect what the mental health status of Chinese rural LBC looks like currently. Third, our search method is somewhat general. The keywords we used to search are only “left-behind children” and “mental health”, which led us to collect only some articles about the related factors and impact mechanisms of the mental health of LBC, so we do not have many studies about the specific mental health issues the LBC often suffer from. Future research could use more specific mental health issues like “depression” or “anxiety” as keywords. Fourth, this study only used a systematic review, which may make the results somewhat subjective. In future research, researchers may need to focus on both urban and rural left-behind children and study more specific mental health issues besides those mentioned in this study. Fifth, almost all the research used was conducted by Chinese scholars, or Chinese scholars accounted for most of the content, so there may be a certain bias in the views. Sixth, for countries where labor force mobility is mainly between countries, the reference value of this study may not be that great. Just like the example of the Philippines, its LBC issue is different from China’s. In China, LBC are mainly children whose parents move between different regions within China, while in the Philippines, LBC are mainly children whose parents move between countries. Although the principles of population movement between countries and between regions within a country are the same, the impacts they cause may be different.
This study researched several common mental health issues that Chinese rural LBC would experience and analyzed the mechanisms by which they affect each other, which can give later studies some hints. Many previous studies have indeed conducted joint analyses of multiple factors and studied the mechanisms by which these factors influence each other, but they rarely analyze more factors together, which is likely to miss the possible effects of some factors that are the subject of the study. For future related research, researchers may consider putting together various LBC mental health issues that previous scholars widely discussed, analyzing how they affect each other, and inferring what kind of mental health issues may be related based on the target factors.
From the perspective of policy, this study has provided a lot of evidence that policies made by countries or societies can really help LBC improve their mental health status and deal with potential mental health issues, while also proving that many problems caused by policies, including irrational resource allocation, will further exacerbate the risks to LBC’s mental health. These can prompt policymakers to consider more about how to create more appropriate policies so that all children, including LBC, can be safer and healthier as they develop. The areas where Chinese rural LBC live are usually less developed than urban areas, which makes it difficult for them to access mental health-related resources and knowledge. At the same time, because the infrastructure conditions in rural areas are usually worse than those in cities, it is difficult for Chinese rural LBC to receive effective treatment if they have mental health problems. Therefore, the national government needs to adopt policies to improve the infrastructure in rural areas, especially the construction of medical facilities, as well as the staffing and quality of medical practitioners. Additionally, the government can even consider providing education and living subsidies to people who migrate from rural areas to work in cities, giving LBC the opportunity to live with their parents in cities, which can reduce some of the risk factors in their lives to a certain extent.
From the perspective of practicality, the interventions and resilience of this study can give social workers, such as educators and community workers, some ideas to help left-behind children. Chinese rural LBC need substantial resources, primarily social resources, to help them deal with the risks of mental health issues. Schools in rural areas need to prioritize the mental health of students, particularly LBC, and educate them about mental health. Society needs to design more intervention programs to provide social support for Chinese rural LBC to help them cope with the risk factors of many mental health issues in life. Besides interventions, LBC do have a certain level of resilience, which can help them resist the mental health risk factors in their lives. However, due to many factors, their resilience also makes them more vulnerable to adverse effects. Relevant practitioners can not only focus on creating new interventions for the mental health of LBC and improving and consolidating existing interventions, but also find ways to stimulate and protect the resilience of LBC themselves. This will be of great reference value in helping them address the mental health issues of LBC.
This study used systematic review methodology to statistically analyze relevant studies, which include the general characteristics of the current situation of Chinese rural LBC’s mental health, related factors of the mental health issues of Chinese rural LBC, Chinese rural LBC’s own resilience towards risk factors for mental health, and how factors like national or social policies and related interventions can help with the mental health of Chinese rural LBC. This study explores the potential relationship among the mental health issues that are very common among LBC. Previous scholars have conducted some similar studies, but not many, and this can prompt scholars or medical staff to consider the possibility of multiple mental health problems occurring simultaneously in LBC and how to address them, as well as provide a method for breaking the links between these problems to avoid the possibility of incomplete treatment intervention. It identified several factors that may pose risks to LBC’s mental health from different aspects, grounding the effects of both macro factors like national or social policies and medical or socio-environmental resources, and micro factors like the resilience of LBC, which can improve their mental health. These insights can inform policymakers on improving and protecting Chinese rural LBC’s mental health, such as increasing resource allocation to rural areas, improving medical and educational facilities, or cultivating high-quality practitioners. Because the issue of LBC is a global topic, and many countries, especially Asian countries, have similar left-behind children’s situations as China, this research can serve as a reference not only for China but also for countries facing similar LBC problems.
Acknowledgement:
Funding Statement: This study is funded by the Fundamental Research Funds for the Central Universities (No. 1233300002).
Author Contributions: The authors confirm contribution to the paper as follows: study conception and design: Jian Li, Yide Chen, Xinyi Zhao, Eryong Xue; data collection: Jian Li, Yide Chen, Xinyi Zhao, Eryong Xue; analysis and interpretation of results: Jian Li, Yide Chen, Xinyi Zhao, Eryong Xue; draft manuscript preparation: Jian Li, Eryong Xue. All authors reviewed and approved the final version of the manuscript.
Availability of Data and Materials: Data available on request from the authors. The data that support the findings of this study are available from Eryong Xue upon reasonable request.
Ethics Approval: This article does not contain any studies with human participants performed by any of the authors.
Conflicts of Interest: The authors declare no conflicts of interest to report.
Supplementary Materials: The supplementary material is available online at https://www.techscience.com/doi/10.32604/ijmhp.2026.073286/s1.
References
1. Tang W , Wang G , Hu T , Dai Q , Xu J , Yang Y , et al. Mental health and psychosocial problems among Chinese left-behind children: a cross-sectional comparative study. J Affect Disord. 2018; 241: 133– 41. doi:10.1016/j.jad.2018.08.017. [Google Scholar] [CrossRef]
2. Wang L , Wei Y , Ma Y , Wang T . Fundamental literature and hot topics on rural left-behind children in China: a bibliometric analysis. Child Care Health Dev. 2016; 42( 6): 852– 8. doi:10.1111/cch.12390. [Google Scholar] [CrossRef]
3. China Development Research Foundation . China Child Development Report 2024: Prioritizing the Development of Children Under New Urbanization. 2024 [cited 2025 Dec 29]. Available from: https://www.cdrf.org.cn/zwcbw/7816.htm. (In Chinese). [Google Scholar]
4. Duan C , Lv L , Guo J , Wang Z . Survival and development of left-behind children in rural China: based on the analysis of the sixth census data. Popul J. 2013; 35( 3): 37– 49. (In Chinese). [Google Scholar]
5. Ren Y , Yang J , Liu L . Social anxiety and Internet addiction among rural left-behind children: the mediating effect of loneliness. Iran J Public Health. 2017; 46( 12): 1659– 68. [Google Scholar]
6. Bögels SM , Alden L , Beidel DC , Clark LA , Pine DS , Stein MB , et al. Social anxiety disorder: questions and answers for the DSM-V. Depress Anxiety. 2010; 27( 2): 168– 89. doi:10.1002/da.20670. [Google Scholar] [CrossRef]
7. Hirsch CR , Meeten F , Krahé C , Reeder C . Resolving ambiguity in emotional disorders: the nature and role of interpretation biases. Annu Rev Clin Psychol. 2016; 12: 281– 305. doi:10.1146/annurev-clinpsy-021815-093436. [Google Scholar] [CrossRef]
8. Schlenker BR , Leary MR . Social anxiety and self-presentation: a conceptualization and model. Psychol Bull. 1982; 92( 3): 641– 69. doi:10.1037/0033-2909.92.3.641. [Google Scholar] [CrossRef]
9. Grant KE , Compas BE , Stuhlmacher AF , Thurm AE , McMahon SD , Halpert JA . Stressors and child and adolescent psychopathology: moving from markers to mechanisms of risk. Psychol Bull. 2003; 129( 3): 447– 66. doi:10.1037/0033-2909.129.3.447. [Google Scholar] [CrossRef]
10. Wang F , Lin L , Lu J , Cai J , Xu J , Zhou X . Mental health and substance use in urban left-behind children in China: a growing problem. Child Youth Serv Rev. 2020; 116: 105135. doi:10.1016/j.childyouth.2020.105135. [Google Scholar] [CrossRef]
11. Marsh HW , Craven RG , McInerney DM . Self-processes, learning, and enabling human potential: dynamic new approaches. Bradford, UK: Emerald Publishing Limited; 2008. p. 269– 88. doi:10.1108/978-1-60752-618-6. [Google Scholar] [CrossRef]
12. Luthans F , Youssef CM , Avolio BJ . Psychological capital: developing the human competitive edge. Oxford, UK: Oxford University Press; 2006. doi:10.1093/acprof:oso/9780195187526.001.0001. [Google Scholar] [CrossRef]
13. Diener E . Subjective well-being. The science of happiness and a proposal for a national index. Am Psychol. 2000; 55( 1): 34– 43. doi:10.1037/0003-066X.55.1.34. [Google Scholar] [CrossRef]
14. Coleman JS . Social capital in the creation of human capital. Am J Sociol. 1988; 94: S95– 120. doi:10.1086/228943. [Google Scholar] [CrossRef]
15. Putnam RD . The prosperous community: social capital and public life. Am Prospect. 1993; Spring: 35– 42. [Google Scholar]
16. Page MJ , McKenzie JE , Bossuyt PM , Boutron I , Hoffmann TC , Mulrow CD , et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021; 372: n71. doi:10.1136/bmj.n71. [Google Scholar] [CrossRef]
17. Critical Appraisal Skills Programme (CASP) . CASP Checklists [Internet]. [cited 2025 Sep 2]. Available from: https://caspuk.net/casp-tools-checklists/. [Google Scholar]
18. Joanna Briggs Institute (JBI) . JBI Critical Appraisal Tools [Internet]. [cited 2025 Sep 2]. Available from: https://jbi.global/critical-appraisal-tools. [Google Scholar]
19. National Collaborating Centre for Methods and Tools (NCCMT) . Mixed Methods Appraisal Tool (MMAT) version 2018 user guide [Internet]. [cited 2025 Sep 2]. Available from: https://www.nccmt.ca/knowledge-repositories/search/232. [Google Scholar]
20. Wang L , Feng Z , Yang G , Yang Y , Dai Q , Hu C , et al. The epidemiological characteristics of depressive symptoms in the left-behind children and adolescents of Chongqing in China. J Affect Disord. 2015; 177: 36– 41. doi:10.1016/j.jad.2015.01.002. [Google Scholar] [CrossRef]
21. Zhang Y , Jiang X , Xiang Y . The development trajectory of depression in left-behind children and the specific effect of different kinships on it: a longitudinal study. Curr Psychol. 2024; 43( 3): 2771– 82. doi:10.1007/s12144-023-04378-7. [Google Scholar] [CrossRef]
22. Shen M , Gao J , Liang Z , Wang Y , Du Y , Stallones L . Parental migration patterns and risk of depression and anxiety disorder among rural children aged 10–18 years in China: a cross-sectional study. BMJ Open. 2015; 5( 12): e007802. doi:10.1136/bmjopen-2015-007802. [Google Scholar] [CrossRef]
23. He B , Fan J , Liu N , Li H , Wang Y , Williams J , et al. Depression risk of ‘left-behind children’ in rural China. Psychiatry Res. 2012; 200( 2–3): 306– 12. doi:10.1016/j.psychres.2012.04.001. [Google Scholar] [CrossRef]
24. Yang F , Shen Y , Nehring D . Maltreatment and depression among left-behind adolescents in rural China: the moderating roles of food security and depression literacy. Child Abuse Negl. 2021; 114: 104976. doi:10.1016/j.chiabu.2021.104976. [Google Scholar] [CrossRef]
25. Ho GWK , Bressington D , Leung SF , Lam KC , Leung AM , Molassiotis A , et al. Depression literacy and health-seeking attitudes in the Western Pacific region: a mixed-methods study. Soc Psychiatry Psychiatr Epidemiol. 2018; 53( 10): 1039– 49. doi:10.1007/s00127-018-1538-6. [Google Scholar] [CrossRef]
26. Bao K , Wu S , Oubibi M , Cai L . Internet gaming disorder among rural left-behind children in China: a sociological qualitative study. Psychol Res Behav Manag. 2025; 18: 387– 403. doi:10.2147/PRBM.S496951. [Google Scholar] [CrossRef]
27. Miao S , Xu L , Gao S , Bai C , Huang Y , Peng B . Internet addiction and suicidal ideation in Chinese children with migrant parents: mediating role of anxiety and moderating role of social support. Acta Psychol. 2024; 248: 104427. doi:10.1016/j.actpsy.2024.104427. [Google Scholar] [CrossRef]
28. Fan X , Huang Y , Yang H , Zhang M , Zhu S , Wen S , et al. Revise the adversity scale for left-behind children in rural China. Chin J Clin Psychol. 2023; 31( 1): 84– 9. (In Chinese). doi:10.16128/j.cnki.1005-3611.2023.01.015. [Google Scholar] [CrossRef]
29. Zhang M , Zhang C , Jiang Z , Liu Y . A latent profile analysis of social anxiety among Chinese left-behind children and adolescents: associations with online parent-child communication and online social capital. Child Abuse Negl. 2024; 158: 107102. doi:10.1016/j.chiabu.2024.107102. [Google Scholar] [CrossRef]
30. Xiao Y , Chen Y , Meng Q , Tian X , He L , Yu Z , et al. Suicide ideation and suicide plan in Chinese left-behind children: prevalence and associated factors. J Affect Disord. 2019; 257: 662– 8. doi:10.1016/j.jad.2019.07.072. [Google Scholar] [CrossRef]
31. Fu M , Xue Y , Zhou W , Yuan TF . Parental absence predicts suicide ideation through emotional disorders. PLoS One. 2017; 12( 12): e0188823. doi:10.1371/journal.pone.0188823. [Google Scholar] [CrossRef]
32. Liu RT , Lawrence HR , Burke TA , Sanzari CM , Levin RY , Maitlin C , et al. Passive and active suicidal ideation among left-behind children in rural China: an evaluation of intrapersonal and interpersonal vulnerability and resilience. Suicide Life Threat Behav. 2021; 51( 6): 1213– 23. doi:10.1111/sltb.12802. [Google Scholar] [CrossRef]
33. Liu LJ , Sun X , Zhang CL , Wang Y , Guo Q . A survey in rural China of parent-absence through migrant working: the impact on their children’s self-concept and loneliness. BMC Public Health. 2010; 10( 1): 32. doi:10.1186/1471-2458-10-32. [Google Scholar] [CrossRef]
34. Ye L , Qian Y , Meng S , Ye D , Rong C , Vandenhouten EE , et al. Subjective well-being of left-behind children: a cross-sectional study in a rural area of Eastern China. Child Adolesc Psychiatry Ment Health. 2020; 14( 1): 27. doi:10.1186/s13034-020-00333-7. [Google Scholar] [CrossRef]
35. Ren Y , Li M , Sun H . Psychological capital status of left-behind rural children in China and its relationship with mental health. Int J Ment Health Promot. 2021; 23( 3): 375– 84. doi:10.32604/ijmhp.2021.014335. [Google Scholar] [CrossRef]
36. Liu Z , Li X , Ge X . Left too early: the effects of age at separation from parents on Chinese rural children’s symptoms of anxiety and depression. Am J Public Health. 2009; 99( 11): 2049– 54. doi:10.2105/AJPH.2008.150474. [Google Scholar] [CrossRef]
37. Liang K , Chen S , Chi X . Care their diet and mind: association between eating habits and mental health in Chinese left-behind children. Nutrients. 2022; 14( 3): 524. doi:10.3390/nu14030524. [Google Scholar] [CrossRef]
38. Wang J , Zou J , Luo J , Liu H , Yang Q , Ouyang Y , et al. Mental health symptoms among rural adolescents with different parental migration experiences: a cross-sectional study in China. Psychiatry Res. 2019; 279: 222– 30. doi:10.1016/j.psychres.2019.03.004. [Google Scholar] [CrossRef]
39. Qi D , Wu L . Different parenting styles and rural children’s mental health: the mediational role of mental resilience. Child Youth Serv Rev. 2024; 163: 107802. doi:10.1016/j.childyouth.2024.107802. [Google Scholar] [CrossRef]
40. Wu Q , Lu D , Kang M . Social capital and the mental health of children in rural China with different experiences of parental migration. Soc Sci Med. 2015; 132: 270– 7. doi:10.1016/j.socscimed.2014.10.050. [Google Scholar] [CrossRef]
41. Han L , Xu W . Communication or alienation? relationship between negative life events and mental health of left-behind children in rural China. Appl Res Qual Life. 2022; 17( 6): 3559– 77. doi:10.1007/s11482-022-10079-3. [Google Scholar] [CrossRef]
42. Xie QW , Zhao G , Lu J , Chen R , Xu J , Wang M , et al. Mental health problems amongst left-behind adolescents in China: serial mediation roles of parent-adolescent communication and school bullying victimisation. Br J Soc Work. 2023; 53( 2): 994– 1018. doi:10.1093/bjsw/bcac168. [Google Scholar] [CrossRef]
43. Gao S , Chan KL , Chen S , Zhong H . Bullying victimization and depression among left-behind adolescents in rural China: roles of hopelessness and grit. Sch Ment Health. 2023; 15( 3): 754– 64. doi:10.1007/s12310-023-09579-w. [Google Scholar] [CrossRef]
44. Wu Y . Comparison of the mental health status of left-behind children before and after the COVID-19 pandemic. Psychol Res Behav Manag. 2023; 16: 5113– 20. doi:10.2147/PRBM.S434897. [Google Scholar] [CrossRef]
45. Hou T , Mao X , Shao X , Liu F , Dong W , Cai W . Suicidality and its associated factors among students in rural China during COVID-19 pandemic: a comparative study of left-behind and non-left-behind children. Front Psychiatry. 2021; 12: 708305. doi:10.3389/fpsyt.2021.708305. [Google Scholar] [CrossRef]
46. Zhang L , Yang F . Food insecurity and school performance among the left-behind children in rural China: depression and educational expectation as mediators. Sch Psychol Int. 2019; 40( 5): 510– 24. doi:10.1177/0143034319869048. [Google Scholar] [CrossRef]
47. Fu Y , Zhou X . Effects of parental migration on Chinese children’s mental health: mediating roles of social support from different sources. Child Fam Soc Work. 2022; 27( 3): 465– 77. doi:10.1111/cfs.12899. [Google Scholar] [CrossRef]
48. Zhao X , Fu F , Zhou L . The mediating mechanism between psychological resilience and mental health among left-behind children in China. Child Youth Serv Rev. 2020; 110: 104686. doi:10.1016/j.childyouth.2019.104686. [Google Scholar] [CrossRef]
49. Guo X , Liu Q , Wang H , Huang K , Lei X , Zhang F , et al. Resilience and its influential factors in left-behind middle school students in Yunyang County of Rural Three Gorges Areas in China: a cross-sectional survey. Public Health. 2015; 129( 11): 1479– 87. doi:10.1016/j.puhe.2015.07.018. [Google Scholar] [CrossRef]
50. Fan X , Lu M . Testing the effect of perceived social support on left-behind children’s mental well-being in mainland China: the mediation role of resilience. Child Youth Serv Rev. 2020; 109: 104695. doi:10.1016/j.childyouth.2019.104695. [Google Scholar] [CrossRef]
51. Man X , Barth RP , Li YE , Wang Z . Exploring the new child protection system in Mainland China: how does it work? Child Youth Serv Rev. 2017; 76: 196– 202. doi:10.1016/j.childyouth.2017.03.012. [Google Scholar] [CrossRef]
52. Sun KS , Lam TP , Cai J , Lam KF , Wu D , Kwok KW , et al. Impact of training on primary care physicians’ management of depression and anxiety disorders in rural China. Int J Soc Psychiatry. 2023; 69( 2): 388– 95. doi:10.1177/00207640221094957. [Google Scholar] [CrossRef]
53. Wang J , Wang X , Li P , Zhang MY , Wu HY , Li DL , et al. Effects of social support and positive psychology intervention on depression and subjective well-being among the left-behind children: a two-year longitudinal study. Curr Psychol. 2023; 42( 34): 30008– 19. doi:10.1007/s12144-022-03783-8. [Google Scholar] [CrossRef]
54. Ren Y , Li M . Influence of physical exercise on social anxiety of left-behind children in rural areas in China: the mediator and moderator role of perceived social support. J Affect Disord. 2020; 266: 223– 9. doi:10.1016/j.jad.2020.01.152. [Google Scholar] [CrossRef]
55. Shang R , Pang H , Jiang J , Ji Y , Liu Q , Zhang M , et al. Internet addiction and depressive and anxious symptoms among Chinese rural left-behind adolescents: mediating roles of resilience and friendship quality. Child Care Health Dev. 2024; 50( 1): e13160. doi:10.1111/cch.13160. [Google Scholar] [CrossRef]
56. Pernia EM . Migration, remittances, poverty and inequality: the Philippines. Quezon City, Philippines: University of the Philippines; 2008. [Google Scholar]
57. Dominguez GB , Hall BJ . The health status and related interventions for children left behind due to parental migration in the Philippines: a scoping review. Lancet Reg Health West Pac. 2022; 28: 100566. doi:10.1016/j.lanwpc.2022.100566. [Google Scholar] [CrossRef]
58. Inter-Agency Standing Committee . IASC guidelines for mental health and psychosocial support in emergency settings. Geneva, Switzerland: World Health Organization; 2007. [Google Scholar]
Cite This Article
 Copyright © 2026 The Author(s). Published by Tech Science Press.
Copyright © 2026 The Author(s). Published by Tech Science Press.This work is licensed under a Creative Commons Attribution 4.0 International License , which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.


 Submit a Paper
Submit a Paper Propose a Special lssue
Propose a Special lssue View Full Text
View Full Text Download PDF
Download PDF Downloads
Downloads
 Citation Tools
Citation Tools