 Open Access
Open Access
ARTICLE
Association between self-compassion, meaning in life, resilience, health-related quality of life and diabetes self-management among people living with type 2 diabetes in Nigeria
1 Faculty of Humanities, North West University, Mahikeng, 2790, South Africa
2 Department of Psychology, University of Nigeria, Nsukka, 410001, Nigeria
* Corresponding Author: Chinenye Joseph Aliche. Email:
Journal of Psychology in Africa 2026, 36(1), 107-115. https://doi.org/10.32604/jpa.2026.075295
Received 29 October 2025; Accepted 12 November 2025; Issue published 26 February 2026
Abstract
Self-compassion is an important psychological resource that improves health-related quality of life and diabetes self-management; however, the psychological processes underlying these associations remain unclear. This study examined the roles of meaning in life and resilience in the relationship between self-compassion and both health-related quality of life and diabetes self-management. Participants were 301 individuals living with type 2 diabetes (176 (58.5%) females, M age = 49.69, SD = 12.36) conveniently selected from two tertiary healthcare institutions in Nigeria. They completed self-report measures of self-compassion, meaning in life, resilience, health-related quality of life and diabetes self-management. Multiple regression analyses indicated that self-compassion positively predicted health-related quality of life and diabetes self-management. Meaning in life and resilience independently and positively predicted health-related quality of life and diabetes self-management. Mediation analysis showed that meaning in life mediated the association between self-compassion and health-related quality of life, as well as diabetes self-management. Likewise, resilience mediated the connection between self-compassion and health-related quality of life, and diabetes self-management behaviour. Intervention for diabetes self-management should focus on promoting self-compassion, meaning in life and resilience abilities of patients, as they can potentially improve health and self-care behaviours needed for recovery.Keywords
Type 2 diabetes mellitus (T2DM) is a major global public health problem of the 21st century (Singer et al., 2022). Over 537 million adults were diagnosed with diabetes in 2021, and the number is projected to rise to 643 and 783 million in 2030 and 2045, respectively (Sun et al., 2022). In Nigeria, over 3.7 million people are living with diabetes mellitus (DM), out of which T2DM constitutes 90 percent of all diabetes cases (Aliche et al., 2023). This chronic disease is associated with long- and short-term complications, high incidence of premature death, and poor health-related quality of life (HRQoL) (Dong et al., 2020; Jeong, 2024; Trikkalinou et al., 2020). In fact, people living with diabetes experience lower HRQoL than the general population (Tietjen et al., 2021). HRQoL reflects the extent to which patients’ happiness and satisfaction with life are impacted by their health condition and treatment (Jeong, 2024). Effective diabetes self-management requires patients to regularly undertake lifelong self-care practices, which include appropriate dietary practices, regular physical activity, self-monitoring of blood glucose, and adherence to prescribed medications (Jafari et al., 2024). Although healthy diabetes self-care behaviours help decrease levels of diabetes distress and promote health maintenance (Jafari et al., 2024), some patients may find certain aspects of diabetes self-management very problematic (Sandham & Deacon, 2023). Thus, to improve patients’ quality of life and diabetes self-management would require self-compassion, a higher sense of meaning in life and related skills (Lazarus & Folkman, 1986; Sandham & Deacon, 2023; Skinner & Kuijer, 2024; Ueno & Amemiya, 2024; Wong & Yeung, 2017). This study examined these relationships in a Nigerian diabetes care setting.
The transactional theory of coping (Lazarus & Folkman, 1986) presents a holistic model of how self-compassion might be linked with meaning-making processes and resilience skills in adaptation to diabetes. According to this theory, stress is not caused by an event itself, but by the individual’s cognitive and behavioural responses to the interaction between a situation and the personal goal, by their primary and secondary appraisal of a life situation or event. The primary appraisal of the event considers the potential threat to their health and quality of life. The secondary appraisal involves personal resources and opportunities needed to deal with the stressful situation (Lazarus & Folkman, 1986). With sufficient personal resources such as optimism and self-compassion that encourage kindness and understanding, potential threats are perceived as more controllable, leading to an increased sense of hope and meaning in life (Lazarus & Folkman, 1986).
Self-compassion as a personal resource might further facilitate adaptive coping responses such as resilience and thus positively influence quality of life and diabetes self-management (Lazarus & Folkman, 1986). For example, individuals high in self-compassion perceive stressful situations as less threatening when considering them in the light of a shared human experience (Neff & Dahm, 2015) and meaningful life experience (Wu et al., 2022). They also would evidence higher levels of resilience when dealing with stressful situations (Ueno & Amemiya, 2024). The current study examines the effect of self-compassion on quality of life and diabetes self-management, and the potential mediating role of meaning in life and resilience.
Self-compassion, quality of life and diabetes self-management
Self-compassion is considered a healthy stance towards the self, or the tendency to profoundly show kindness, care and love to oneself in the face of adversity (Garcia et al., 2021). According to Neff (2003)’s model, self-compassion involves three critical components: self-kindness vs. self-judgement, common humanity vs. isolation, and mindfulness vs. over-identification. Self-kindness captures the willingness to provide oneself with support, warmth and understanding instead of rendering harsh criticisms to oneself. Common humanity involves the acknowledgement that suffering is an integral part of human life. Mindfulness captures the tendency to be aware of one’s sufferings with clarity and balanced perspectives without over-identifying with negative emotions and thoughts (Neff, 2003). Self-compassion is consistently associated with multiple indicators of positive psychological outcome, including the intention to seek prompt medical care (Sandham & Deacon, 2023), better physical health and improved HRQoL (Garcia et al., 2021; Kauser et al., 2022; Skinner & Kuijer, 2024). Self-compassion helps to promote clinical outcomes (Misurya et al., 2020) and diabetes self-care behaviours (Loseby et al., 2022). Additionally, Sandham and Deacon (2023) provided evidence for the positive effect of self-compassion on diabetes self-management. This underscores the positive effect of self-compassion in improving diabetes self-management and HRQoL.
Researchers have proposed that a greater ability to find meaning in life (MIL) may conveniently convey the positive effect of self-compassion on health outcomes (Zipagan & Galvez Tan, 2023). MIL refers to an individual’s feeling of having an objective in life, and consistently working towards achieving it (Zipagan & Galvez Tan, 2023). For individuals living with a chronic health condition, MIL is considered an important positive psychological attribute that can help to cope with the stressful situation. MIL is positively related to posttraumatic growth (Aliche et al., 2019) and HRQoL (Barsaei et al., 2020; Kim et al., 2019). MIL is a major source of motivation to engage in self-care behaviours that are personally valued and cherished (Hu & Lu, 2024; Kang et al., 2021; Nie et al., 2023). As such, type 2 diabetes patients with a higher sense of meaning in life experience lower levels of death anxiety, avoidance behaviour and better adjustment with diabetes (Aliche et al., 2023). Crucially, substantial evidence revealed the mediating effect of meaning in life in the association of self-compassion and better health outcomes (Wong & Yeung, 2017; Wu et al., 2022; Zipagan & Galvez Tan, 2023).
Resilience is another psychological resource that is essential in coping with daily stresses that come with diabetes (Parviniannasab et al., 2024). It is defined as the capacity to withstand difficulties and overcome life challenges (Jia et al., 2022). Resilience is robustly identified as a protective factor of wellbeing and quality of life of people with a medical condition (Afeera et al., 2022; Cheng et al., 2024; Qiu et al., 2019). Due to increasing recognition that individuals with diabetes require lifelong adherence to self-management behaviour, researchers and healthcare practitioners have strongly identified resilience as an important factor that influences adherence to diabetes self-management (Jia et al., 2022; Wang et al., 2023; Wilson et al., 2017). Self-compassion can fundamentally contribute to improved resilience, which then buffers individuals against negative mental health outcomes with resilience (Jia et al., 2022; Ueno & Amemiya, 2024). Robust evidence revealed that resilience plays a mediating role in the association of self-compassion and health outcome (Ma & Xiao, 2024; Pérez-Aranda et al., 2021; Ueno & Amemiya, 2024). Few studies have simultaneously explored the relationship between self-compassion, meaning in life, resilience, HRQoL and diabetes self-management among T2DM patients.
Goals of the study. This study aims to examine whether the association between HRQoL, diabetes self-management and self-compassion would be mediated by meaning in life and resilience. Figure 1 presents the study’s conceptual model regarding HRQoL and diabetes self-management.
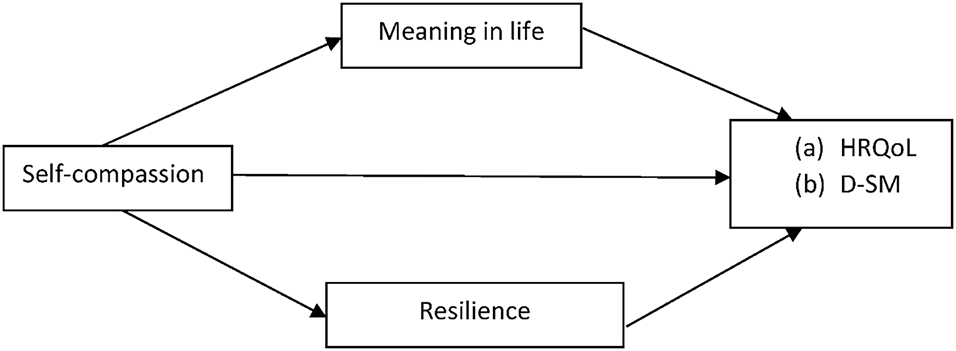
Figure 1: The conceptual model. Note. HRQoL = Health-related quality of life; D-SM = Diabetes self-management.
Following Figure 1, we hypothesized that:
Hypothesis 1: Self-compassion is associated with improved HRQoL and diabetes self-management.
Hypothesis 2: Meaning in life is associated with improved HRQoL and diabetes self-management.
Hypothesis 3: Resilience is associated with improved HRQoL and diabetes self-management.
Hypothesis 4: Meaning in life would mediate the association between self-compassion and HRQoL/diabetes self-management, such that patients with higher self-compassion experience a greater sense of meaning in life, which leads to improved HRQoL and diabetes self-management.
Hypothesis 5: Resilience would mediate the association between self-compassion and HRQoL/diabetes self-management, such that patients with higher self-compassion experience higher resilience for improved HRQoL and diabetes self-management.
Participants consisted of 301 people living with type 2 diabetes who were conveniently selected from the outpatient unit of two tertiary healthcare institutions in Nigeria. Inclusion criteria were: an adult (>18 years), having a confirmed diagnosis of type 2 diabetes, conscious and mentally stable to be able to respond to the psychological instrument independently or with the help of research assistants, having the ability to read and understand English language at least at high school level, and not taken any antipsychotic medication as at the period of this study or having any neurological disorders.
Self-compassion. Self-compassion was measured using the 12-item Self-Compassion Scale–Short Form (Raes et al., 2011). The items (e.g., “when I am going through a very bad time, I give myself the caring and tenderness I need”) are rated on a 5-point response scale ranging from 1 (almost never) to 5 (almost always). Items are reverse-scored where necessary, with scale scores ranging from 12 to 60, and higher scores indicating greater self-compassion. There is evidence that the short form correlates almost perfectly well with the original, longer version of the scale and shows a good internal consistency reliability coefficient value of 0.85 (Raes et al., 2011). In the present study, a reliability coefficient alpha of 0.82 was obtained.
Meaning in life. Meaning in life was measured using the 5-item presence of meaning in life subscale of the Meaning in Life Questionnaire (MLQ) (Steger et al., 2006). The items (‘I have a good sense of what makes my life meaningful’) are scored on a 7-point Likert scale ranging from 1 (absolutely untrue) to 7 (absolutely true), with a higher score representing a greater sense of meaning in life. The developers reported good validity and reliability indices for the scale with an internal consistency reliability coefficient value of 0.88 (Steger et al., 2006). In the present study, we obtained a Cronbach’s alpha coefficient value of 0.81.
Resilience. Resilience was measured using the 14-item resilience scale (RS; Wagnild & Young, 1993). Items (“I think of myself as a strong person when facing challenges”) are scored on a 7-point Likert scale ranging from (1) Strongly disagree to (7) Strongly agree, with total scores ranging from 14 to 98 and higher scores indicating greater resilience ability. The RS has excellent psychometric properties with a reliability coefficient of 0.91 observed in a wide range of studies; concurrent validity observed with morality (0.31), life satisfaction (0.37), self-reported health status (0.30), depression (−0.41) and the longer 25-item resilience scale (0.97) (Wagnild & Young, 1993). In this study, we obtained a Cronbach’s alpha reliability coefficient of 0.79.
Health related quality of life (HRQoL). HRQoL was assessed with the 15-item short form of the Diabetes Quality of Life Questionnaire (DQOLQ) that was derived from the original 60-item DQOLQ (Burroughs et al., 2004). The items (e.g., “How satisfied are you with the amount of time it takes you to manage your diabetes”) are scored on a 5-point Likert scale ranging from 1 (very satisfied) to 5 (very dissatisfied), with lower scores suggesting improved diabetes-related quality of life. The DQOLQ has excellent validity with an internal consistency reliability coefficient of 0.85 and a test-retest reliability of 0.513. The scale has demonstrated a good convergent validity, having strongly correlated with the original 60-item DQOLQ full scale (r = 0.91), alongside the individual DQOLQ subscales: social worry subscale (r = 0.52), and satisfaction with diabetes control subscale (r = 0.97). This study obtained an alpha coefficient value of 0.83.
Diabetes self-management behaviour. Diabetes self-management behaviour was measured using the 16-item Diabetes Self-Management Questionnaire (DSMQ) (Schmitt et al., 2013). The items of DSMQ cover five different aspects of diabetes self-management: dietary control (DC), physical activity (PA), glucose management (GM) and health-care use (HU). The items (e.g., ‘I keep all doctor’s appointments recommended for my diabetes treatment’) are scored using a 4 point Likert scale from 0 = (does not apply to me) to 3 = (applies to me very much), and item scores are summed and transformed into a scale ranging from 0 to 10 (for details, see: Schmitt et al., 2013). Higher scores indicate greater adherence to diabetes self-management behaviours. The DSMQ showed strong convergent validity and an internal consistency reliability coefficient value of 0.84 for the sum scale. The present study obtained a reliability coefficient value of 0.82.
After obtaining ethical approval from the Research Ethical Committee of the University of Nigeria Teaching Hospital, Ituku-ozala, Enugu State, Nigeria (Ethics Clearance Number: NHREC/59/10/05/2024), data collection commenced with the help of two trained research assistants. Informed consent was obtained from all participants before participation. They were also informed about the confidentiality of their responses, as their feedback is anonymous and no identifying data will be collected. They are free to withdraw from the study at any stage.
Descriptive statistics were used to carry out a preliminary analysis. Pearson’s correlation was employed to examine the association between the demographic variables (e.g., age, gender, and time since T2DM diagnosis) and the main study variables. Multiple regression, using the step-wise method, was employed to establish baseline association among the demographics (e.g., age, gender, and time since T2DM diagnosis) and the main study variables. Hayes PROCESS macro for SPSS Model 4 was used for the mediation analysis.
Two parallel mediation models were tested in this study. In the first model, self-compassion was the independent variable, meaning in life and resilience were mediator variables, and health-related quality of life was the dependent variable (Figure 1a). In the second model, self-compassion was the independent variable, meaning in life and resilience were mediator variables, and diabetes self-management was the dependent variable (Figure 1b). The covariates (age, gender and time since diagnosis) were not included in the mediation models because they were not significantly corrected with any of the study variables. Multicollinearity was tested by examining Tolerance and Variable Inflation Factor (VIF): Tolerance values below 0.20 (Menard, 1995) and VIF above 5.0 (James et al., 2013) were considered indicators of multicollinearity issues. The 95% bootstrap confidence intervals CI were calculated using 5000 bootstrapped samples, and significant results were affirmed if the 95%CI did not include zero between the straddles (Hayes, 2018). All the data analysis was carried out using the Statistical Packages for Social Sciences (SPSS), version 23.
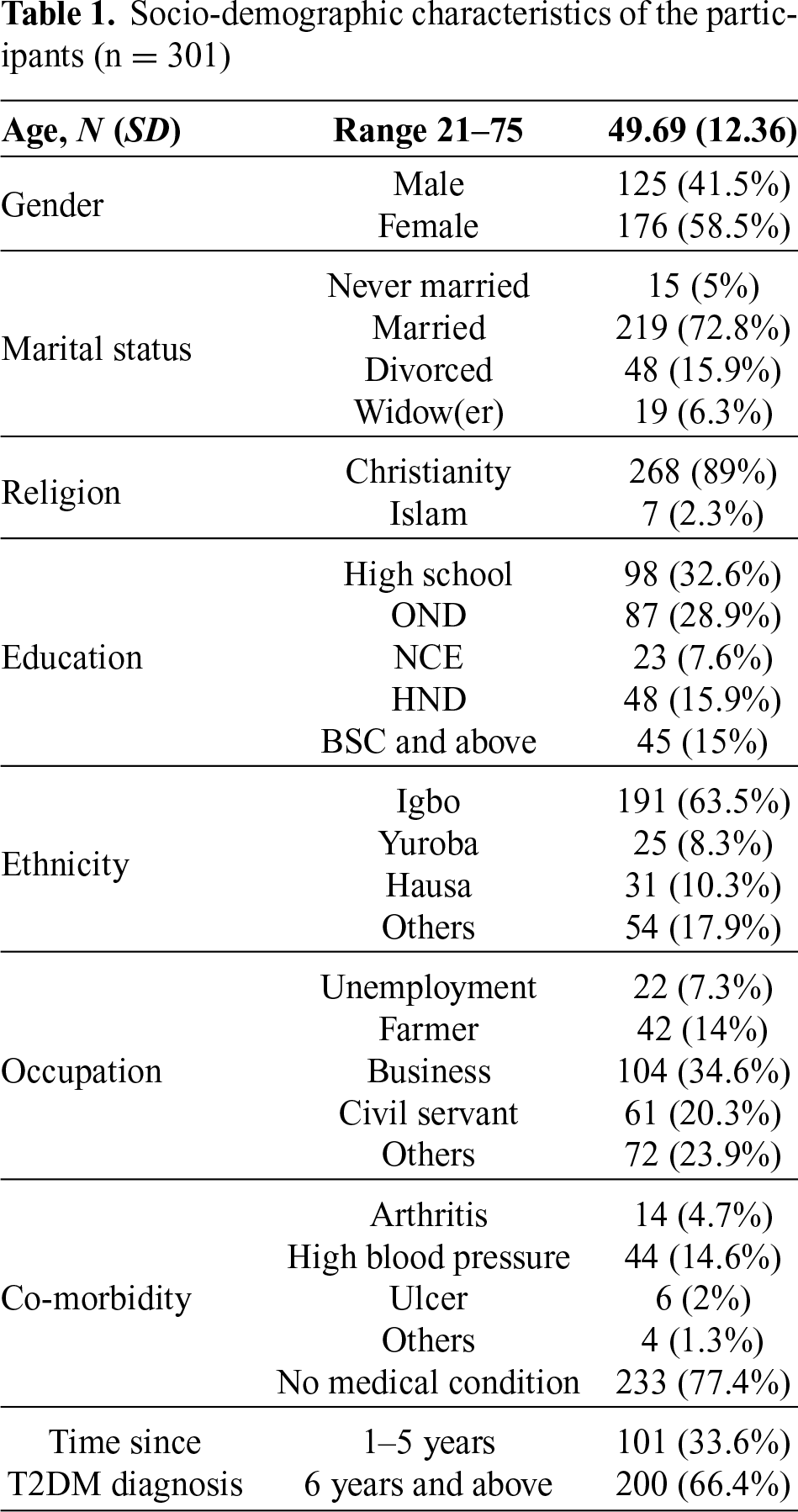
The socio-demographic characteristics of the participants are presented in Table 1. Results showed that the age of participants ranged from 21 to 75 years (Mean = 49.69, SD = 12.36). The majority were female (n = 176, 58.5%), who were married (n = 219, 72.8%), and their religion was Christianity (n = 268, 89%). Most of them had a high school education (n = 98, 32.6%) and were from the Igbo ethnic group (n = 191, 63.5%). They were predominantly doing business as their occupation (n = 104, 34.6%) with no underlined medical condition or co-morbidity (n = 233, 77.4%). Regarding the time since T2DM diagnosis, the majority were between 6 to 10 years (n = 200, 66.4%).
Pearson correlation results (see Table 2) showed that the demographic variables (age, gender and time since T2DM diagnosis) were not significantly correlated with the main study variables. SC positively correlated with MIL (r = 0.13, p < 0.01), resilience (r = 0.22, p < 0.001), HRQoL (r = 0.15, p < 0.01) and D-SM (r = 0.12, p < 0.05). MIL positively correlated with resilience (r = 0.44, p < 0.001), HRQoL (r = 0.48, p < 0.001) and D-SM (r = 0.48, p < 0.001). Resilience correlated positively with HRQoL (r = 0.59, p < 0.001) and D-SM (r = 0.51, p < 0.001), whereas HRQoL and D-SM were positively correlated with each other (r = 0.67, p < 0.001).

Relationship between demographic variables, self-compassion, meaning in life, resilience, health-related quality of life and diabetes self-management.
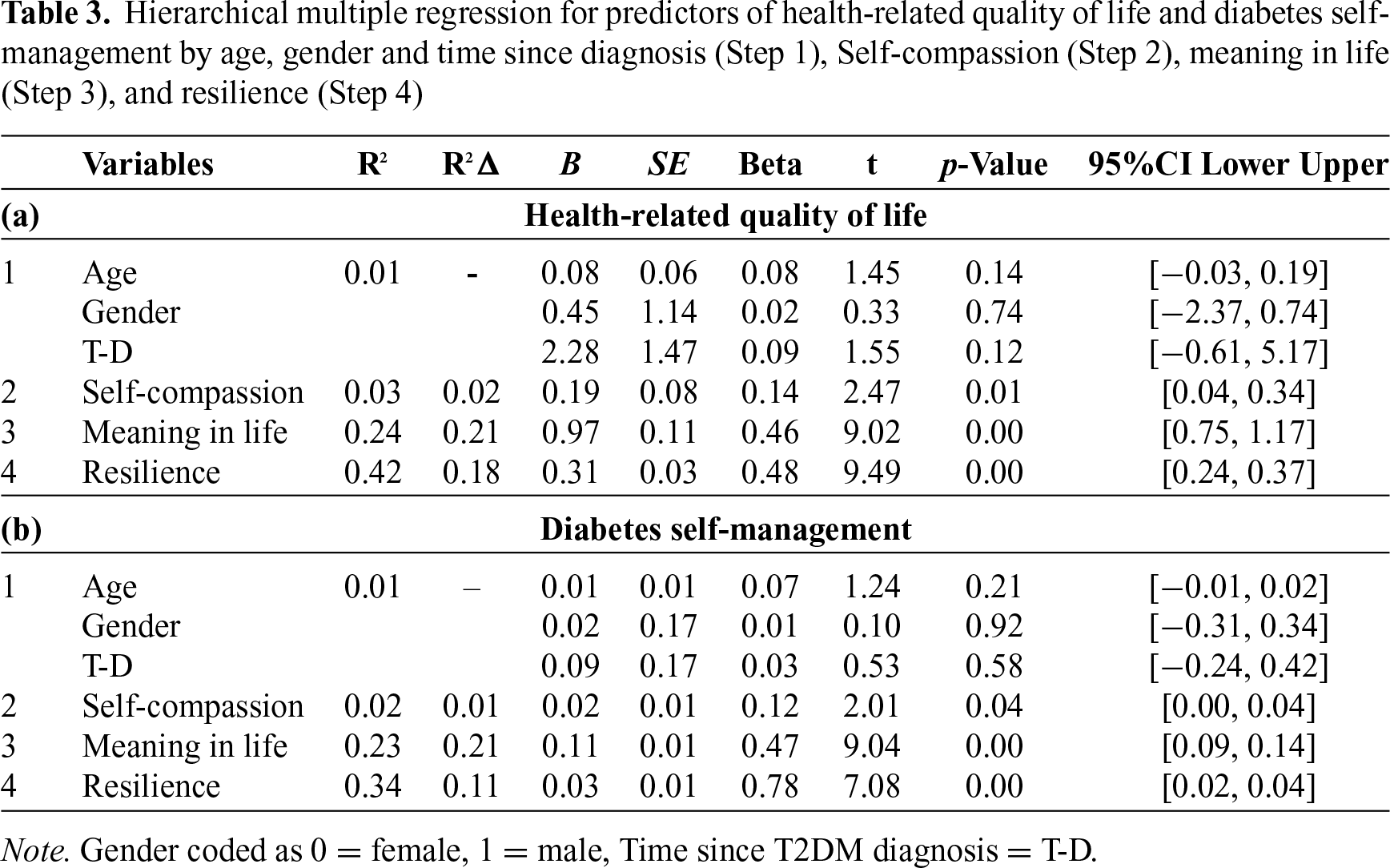
To understand the relationship among the study variables, two hierarchical multiple regression analysis were conducted using health-related quality of life and diabetes self-management as dependent variables (See Table 3). In each regression analysis, demographic variable (age, gender and time since T3DM diagnosis) was entered into step 1, self-compassion in step 2, meaning in life in step 3 and resilience in step 4. Results indicated that the demographic variables as a whole did not contribute significantly to the variance in quality of life, R2 = 0.01, F (3, 297) = 1.397, p > 0.05. Self-compassion accounted for a significant amount of variance in quality of life, R2Δ = 0.02, ΔF (1, 296) = 6.112, p < 0.05. Meaning in life and resilience were independent and significant predictors of quality of life, R2Δ = 0.21, ΔF (1, 295) = 81.361, p < 0.001; R2Δ = 0.18, ΔF (1, 294) = 90.118, p < 0.001. When diabetes self-management was considered as a criterion variable in the second model, results showed that the demographic variables did not contribute to the variance in diabetes self-management, R2 = 0.01, F (3, 297) = 0.588, p > 0.05. Self-compassion accounted for a significant amount of variance in diabetes self-management, R2Δ = 0.01, ΔF (1, 296) = 4.047, p < 0.05. Meaning in life explained an additional 21% of the variance in diabetes self-management, R2Δ = 0.21, ΔF (1, 295) = 81.753, p < 0.001. The inclusion of resilience accounted for an increase in variance in diabetes self-management, R2Δ = 0.11, ΔF (1, 294) = 50.049, p < 0.001 (Hypotheses 1, 2 and 3 are supported).
The first mediation model (Figure 2) investigates the mediating role of MIL and resilience in the relationship between self-compassion and HRQoL. Results revealed that self-compassion showed a significant and positive total effect on HRQoL (β = 0.20, t = 2.70, p < 0.05), and the model was significant, F (1, 299) = 7.29, p < 0.01, R2 = 0.24. Furthermore, self-compassion was positively associated with PML (β = 0.08, t = 2.29, p < 0.05), and the model was significant, F (1, 299) = 5.26, p < 0.0.05, R2 = 0.02. Self-compassion was also positively associated with resilience (β = 0.45, t = 3.82, p < 0.001), and the model was significant, F (1, 299) = 14.57, p < 0.001, R2 = 0.045. When the mediators (MIL and resilience) were added to the model, the previously significant association between self-compassion and HRQoL was no longer significant (β = 0.02, t = 0.37, p > 0.05). Meanwhile, PML was positively associated with HRQoL (β = 0.55, t = 5.31, p < 0.001). Resilience was positively associated with HRQoL (β = 0.31, t = 9.49, p < 0.001). The overall model was significant, F (3, 297) = 69.538, p < 0.001, R2 = 0.41. The 95% bias-corrected confidence interval based on 5000 bootstrap samples indicated that the completely standardised indirect effect was significant (self-compassion-PML-HRQoL: Effect = 0.035, SE = 0.02, 95%CI: 0.01 to 0.07); (self-compassion-Resilience-HRQoL: Effect = 0.10, SE = 0.03, 95%CI: 0.04 to 0.17). These findings indicated that PML and resilience independently mediated the association between self-compassion and HRQoL as the 95%CI did not contain zero in between the upper and lower confidence intervals.
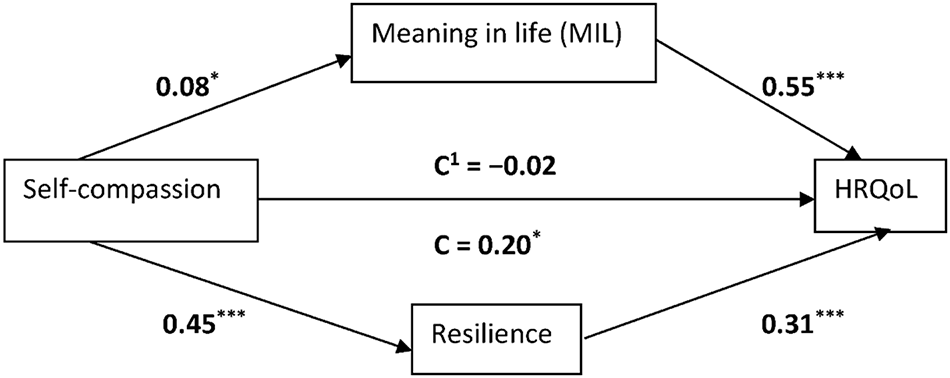
Figure 2: Graphical representation of the mediation effect of meaning in life and resilience in the relationship between self-compassion and health-related quality of life. Note. *p < 0.05; ***p < 0.001.
Figure 3 presents the results on the mediating role of MIL and resilience in the association between self-compassion and D-SM. We found that self-compassion showed a significant and positive total effect on D-SM (β = 0.02, t = 2.16, p < 0.05), and the model was significant, F (1, 299) = 4.67, p < 0.05, R2 = 0.02. Self-compassion was positively associated with MIL (β = 0.08, t = 2.29, p < 0.05), and the model was significant, F (1, 299) = 5.26, p < 0.05, R2 = 0.02. Self-compassion was positively related to resilience (β = 0.45, t = 3.82, p < 0.001), and the model was significant, F (1, 299) = 14.57, p < 0.001, R2 = 0.05. The addition of the mediators (MIL and resilience) to the model led to a non-significant association between self-compassion and D-SM (β = 0.01, t = 0.04, p > 0.05). MIL was positively associated with D-SM (β = 0.07, t = 5.91, p < 0.001). Resilience was positively related to D-SM (β = 0.03, t = 7.08, p < 0.001), and the overall model was significant, F (3, 297) = 51.33, p < 0.001, R2 = 0.34. The completely standardised indirect effect supported a significant mediation (Self-compassion-PML-D-SMB: Effect = 0.04, SE = 0.02, 95%CI: 0.01 to 0.08) (Self-Compassion-Resilience-D-SMB: Effect = 0.08, SE = 0.03, 95%CI: 0.03 to 0.15). These results indicate that MIL and resilience are independent mechanisms through which self-compassion promotes D-SMB. However, resilience has the strongest mediation effect on the relationship between self-compassion and D-SM (Hypotheses 4 and 5 are supported).
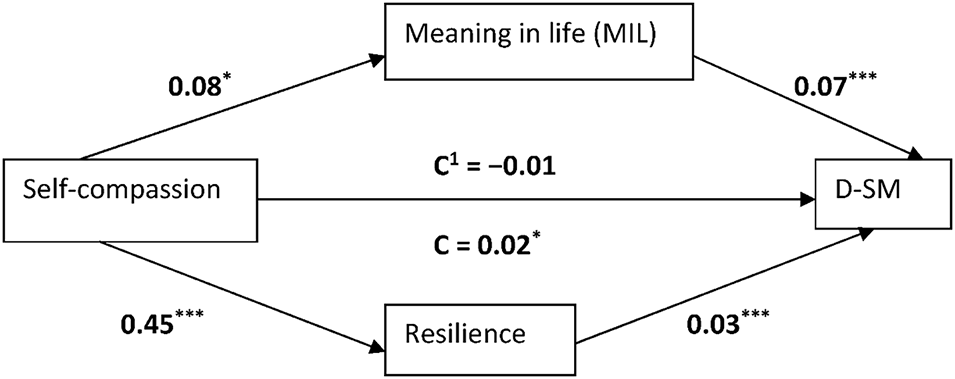
Figure 3: Graphical representation of the mediation effect of meaning in life and resilience in the relationship between self-compassion and diabetes self-management. Note: *p < 0.05; ***p < 0.001
The current study examined the relationship between self-compassion, meaning in life, resilience, HRQoL and diabetes self-management. The results revealed that meaning in life mediated the association of self-compassion, HRQoL and diabetes self-management. This suggests that diabetes patients with a higher self-compassionate attitude experienced improved HRQoL and reported higher engagement in diabetes self-management through a greater sense of meaning in life. Consistent with prior studies (Kauser et al., 2022; Sandham & Deacon, 2023), this study found a positive association between self-compassion, HRQoL and diabetes self-management. Diabetic patients with higher self-compassion treat themselves with kindness while enduring diabetes-related stress, and this helps to improve HRQoL and wellbeing. The friendly attitude towards self (self-compassion) enables patients to comfortably, engage in effective, healthy eating habits, regular physical exercise, adherence to medications and close management of blood glucose levels. Indeed, diabetic patients who show compassion to themselves have the capacity to forgive themselves and engage with their suffering instead of avoiding it (Loseby et al., 2022). This kind of treatment to oneself helps to promote wellbeing, quality of life and facilitates the desire to engage in diabetes health behaviours.
Having acknowledged that illness is a universal phenomenon that anyone can experience, and developing an increased willingness to care for oneself, patients are afforded more opportunity to make meaning out of their life challenges (Zipagan & Galvez Tan, 2023). Additionally, diabetes patients who see their negative life experiences from a balanced perspective, without magnifying and over-identifying with them (mindfulness), are able to process their experience in a healthy manner and in ways that make more positive meaning to them (Wong & Yeung, 2017). This higher sense of life meaning helps to improve HRQoL and the willingness to effectively practice diabetes self-management. Therefore, the findings on the mediating effect of meaning in life in the connection between self-compassion, HRQoL and diabetes self-management behaviour, not only corroborate previous related studies (Wong & Yeung, 2017; Zipagan & Galvez Tan, 2023), but are further considered very critical to the development of interventions to promote the health and wellbeing of diabetes patients. Self-compassion can function as a protective factor by alleviating negative emotions and diabetes related distress that may impede healing and health maintenance. With this, patients are more able to process their health-related issues adaptively, leading to more clarity and a higher sense of meaning in life. This, in turn, encourages people to attach more value to life goals and aspirations, ultimately leading to more engagement in diabetes self-management and improving HRQoL.
Furthermore, results showed that resilience mediated the association between self-compassion, HRQoL and diabetes self-management. In other words, diabetes patients with a higher self-compassion exhibited higher level of resilience, which leads to better HRQoL and increased willingness to engage in diabetes self-management behaviour. This finding aligns with previous studies revealing the mediating effect of resilience on self-compassion and health outcomes (Ma & Xiao, 2024; Pérez-Aranda et al., 2021). Self-compassion fosters the expansion of cognitive changes associated with increased resilience, ultimately resulting in improved HRQoL and diabetes self-care behaviours. This explains why most resilience intervention approaches are anchored on cognitive behaviour therapy that focuses on the patients’ cognitive processes (Liu et al., 2020). Being self-compassionate to oneself enables people to develop resilience (Ueno & Amemiya, 2024). Crucially, certain life experiences can expose individuals to multiple psychological crises and deep misfortune. Such a life experience can prepare some individuals to withstand multiple psychological crises while making others collapse in the face of any slight ordeal. Some individuals emerge to be stronger than others who were also exposed to the same ordeal. Resilience is that psychosocial factor that accounts for the marked difference. Resilience enables people to bounce back and adjust adequately to challenging situations (Cheng et al., 2024). In the context of diabetes, resilience enables patients to adapt and perform optimally to overcome psychological and emotional distress, making it very critical in promoting health behaviour and HRQoL (Parviniannasab et al., 2024). Generally, resilience is the foundation of the diabetes patients’ positive mental health (Jia et al., 2022) and the heart of resilience lies in the individual’s attitude to self. As self-compassion helps patients to cope with painful situations, being compassionate is meaningfully associated with more optimal clinical, behavioural, and positive psychological outcomes in people with diabetes through the mechanism of increased resilience. Based on these findings, it is essential that interventions to promote self-care management and HRQoL of T2DM patients target their self-compassionate attitude and resilience abilities.
Clinical interventions aimed to promote HRQoL and diabetes self-management among type 2 diabetic patients should be holistic, incorporating the services of different health professionals, including medical doctors, nurses and clinical psychologists. Such intervention should focus on simultaneously facilitating self-compassion, meaning in life and resilient skills of patients. The Self-Compassion-based intervention, such as the Mindful Self-compassion Intervention Program (Neff & Germer, 2018) may thus be blended with Logotherapy (FrankL, 1959) for meaning in life; and the resilience intervention based on cognitive behavioural therapy (Liu et al., 2020) for promoting resilience abilities of patients. There is evidence to suggest that these interventions have been beneficial in reducing distress and promoting wellbeing and diabetes self-management among people living with diabetes (Dubois et al., 2020; Friis et al., 2016; Shabani & Mahmoudi Tabar, 2021; Visagie et al., 2023). Implementing these interventions may begin with the assessment of patients’ levels of self-compassion, meaning in life, resilience, HRQoL and diabetes self-management. Diabetic patients who had below-average scores in any or all of the scales should be the prime target of the intervention.
Limitations of the study and future directions
Despite these novel contributions, this research has notable limitations that should be acknowledged when interpreting the findings. Firstly, the cross-sectional nature of the study only establishes association among variables, not causality. Future experimental or longitudinal studies are needed to establish causality among the variables. Secondly, this research focuses on self-compassion, meaning in life and resilience as factors influencing HRQoL and diabetes self-management. Future research should consider exploring other psychosocial factors, such as mindfulness, distress tolerance, coping strategies, as well as physiological factors that may contribute to health and disease maintenance. Finally, this research relied solely on self-report measures in the data collection, which might introduce unknown social desirability biases, and future studies should utilize observational data.
The current study has made a valuable contribution to understanding the role of psychosocial factors in T2DM management with strong methodological foundations. Specifically, it provided preliminary evidence on the mediating role of meaning in life and resilience in the connection between self-compassion, HRQoL, with diabetes self-management. With meaning in life and resilience as independent pathways, diabetes patients can maximise the potential benefit of self-compassion intervention by promoting resilience abilities and helping individuals derive a sense of meaning out of their painful circumstances. The results provide initial insights as to how self-compassion may promote HRQoL and diabetes self-care management. Based on these findings, healthcare providers should prioritise interventions that promote self-compassion, meaning in life and resilience of patients to improve their HRQoL with diabetes self-management.
Acknowledgement: Not applicable.
Funding Statement: The authors received no specific funding for this study.
Author Contributions: Chinenye Joseph Aliche: Conceptualization, Methodology, Material preparation, Data collection, Statistical analyses, Writing—original draft preparation, Subsequent drafts, Reviewing, Editing and statistical analyses. Erhabor Sunday Idemudia: Writing—contributions to later drafts, Reviewing, Editing. Ike E. Onyishi: Methodology, Data collection, Reviewing and editing. All authors reviewed and approved the final version of the manuscript.
Availability of Data and Materials: The datasets generated and analyzed during the current study are available from the corresponding author on reasonable request.
Ethics Approval: The study obtained ethical approval from the Research Ethical Committee of University of Nigeria Teaching Hospital, Ituku-ozala, Enugu State, Nigeria (Ethics Clearance Number: NHREC/59/10/05/2024), data collection commenced with the help of two trained research assistants.
Informed Consent: Informed consent was obtained from all participants before participation.
Conflicts of Interest: The authors declare no conflicts of interest to report regarding the present study.
References
Afeera, U. Z., Ateeq, M. M. J., Azhar, K. J., & Yunus, R. M. (2022). Resilience and health-related quality of life among hepatitis C patients in Pahang, Malaysia.Bangladesh Journal of Medical Science, 21(1), 165–170. https://doi.org/10.3329/bjms.v21i1.56344. [Google Scholar] [CrossRef]
Aliche, C. J., Ifeagwazi, C. M., & Ezaka, E. S. (2023). Moderating role of meaning in life in the relationship of death anxiety, experiential avoidance and health-related quality of life among type 2 diabetes patients. South African Journal of Psychology, 53(4), 533–547. https://doi.org/10.1177/00812463231186328 [Google Scholar] [CrossRef]
Aliche, J. C., Ifeagwazi, C. M., Onyishi, I. E., & Mefoh, P. C. (2019). Presence of meaning in life mediates the relations between social support, posttraumatic growth, and resilience in young adult survivors of a terror attack. Journal of Loss & Trauma, 24(8), 736–749. https://doi.org/10.1080/15325024.2019.1624416 [Google Scholar] [CrossRef]
Barsaei, M., Feizollahzadeh, H., Jabbarzadeh, F., Hasankhani, H., & Shabanloei, R. (2020). The meaning of life related to heart disease and its relationship to quality of life after repeat coronary artery angioplasty. Creative Nursing, 26(1), 48–55. https://doi.org/10.1891/1078-4535.26.1.48. [Google Scholar] [PubMed] [CrossRef]
Burroughs, T. E., Desikan, R., Waterman, B. M., Gilin, D., & McGill, J. (2004). Development and validation of the diabetes quality of life brief clinical inventory. Diabetes Spectrum, 17(1), 41–49. https://doi.org/10.2337/diaspect.17.1.41 [Google Scholar] [CrossRef]
Cheng, C. -H., Hsu, C. -H., Sie, J. -R., Tsay, S. -L., & Tung, H. -H. (2024). The relationship between resilience and healthrelated quality of life among heart failure patients in new york heart association functional classes II and III. Journal of Nursing Research, 32(1), e312. https://doi.org/10.1097/jnr.0000000000000594. [Google Scholar] [PubMed] [CrossRef]
Dong, D., Lou, P., Wang, J., Zhang, P., Sun, J. et al. (2020). Interaction of sleep quality and anxiety on quality of life in individuals with type 2 diabetes mellitus. Health and Quality of Life Outcomes, 18(1), 137. https://doi.org/10.1186/s12955-020-01406-z. [Google Scholar] [PubMed] [CrossRef]
Dubois, S. K., Lehrer, H. M., Whyne, E. Z., & Steinhardt, M. A. A. (2020). Resilience intervention for adults with type 2 diabetes: Proof-of-concept in community health centers. International Journal of Behaviourial Medicine, 27(5), 565–575. https://doi.org/10.1007/s12529-020-09894-5. [Google Scholar] [PubMed] [CrossRef]
Frankl, V. (1959). Man’s search for meaning. Boston, MA, USA: Beacon Press. [Google Scholar]
Friis, A. M., Johnson, M. H., Cutfield, R. G., & Consedine, N. S. (2016). Kindness matters: A randomized controlled trial of a mindful self-compassion intervention improves depression, distress, and HbA1c among patients with diabetes. Diabetes Care, 39(11), 1963–1971. https://doi.org/10.2337/dc16-0416. [Google Scholar] [PubMed] [CrossRef]
Garcia, A. C. M., Camargos Junior, J. B., Sarto, K. K., Marcelo, C. A. D. S., Paiva, E. M. D. C. et al. (2021). Quality of life, self-compassion and mindfulness in cancer patients undergoing chemotherapy: A cross-sectional study. European Journal of Oncology Nursing, 51(4), 101924. https://doi.org/10.1016/j.ejon.2021.101924. [Google Scholar] [PubMed] [CrossRef]
Hayes, A. F. (2018). Introduction to mediation, moderation, and conditional process analysis: A regression-based approach. New York, NY, USA: The Guilford Press. [Google Scholar]
Hu, Y., & Lu, W. (2024). Meaning in life and health behavior habits during the COVID-19 pandemic: Mediating role of health values and moderating role of conscientiousness. Current Psychology, 43(16), 14935–14943. https://doi.org/10.1007/s12144-022-04020-y. [Google Scholar] [PubMed] [CrossRef]
Jafari, A., Naddafi, F., Gholian-Aval, M., & Tehrani, H. (2024). Relationship between diabetes health literacy, distress, burnout, social support, complications, self-care behaviors, and quality of life among patients with type 2 diabetes: A path analysis study. Diabetology & Metabolic Syndrome, 16(1), 248. https://doi.org/10.1186/s13098-024-01391-z. [Google Scholar] [PubMed] [CrossRef]
James, G., Witten, D., Hastie, T., & Tibshirani, R. (2013). An introduction to statistical learning (Vol. 112, pp. 18), New York, NY, USA: springer. https://doi.org/10.1007/978-1-4614-7138-7. [Google Scholar] [CrossRef]
Jeong, M. (2024). Associations of sleep quality and physical activity with diabetes quality of life in korean americans with type 2 diabetes: A cross-sectional study. Healthcare, 12(7), 756. https://doi.org/10.3390/healthcare12070756. [Google Scholar] [PubMed] [CrossRef]
Jia, J., Jenkins, A. J., Quintiliani, L. M., Truong, V., & Lasser, K. E. (2022). Resilience and diabetes self-management among African-American men receiving primary care at an urban safety-net hospital: A cross-sectional survey. Ethnicity & Health, 27(5), 1178–1187. https://doi.org/10.1080/13557858.2020.1849566. [Google Scholar] [PubMed] [CrossRef]
Kang, Y., Cosme, D., Pei, R., Pandey, P., Carreras-Tartak, J. et al. (2021). Purpose in life, loneliness,and protective health behaviors during the COVID-19 pandemic. The Gerontologist, 61(6), 878–887. https://doi.org/10.1093/geront/gnab081. [Google Scholar] [PubMed] [CrossRef]
Kauser, S., Keyte, R., Regan, A., Nash, E. F., Fitch, G. et al. (2022). Exploring associations between self-compassion, self-criticism, mental health, and quality of life in adults with cystic fibrosis: Informing future interventions. Journal of Clinical Psychology in Medical Settings, 29(2), 332–343. https://doi.org/10.1007/s10880-021-09831-y. [Google Scholar] [PubMed] [CrossRef]
Kim, J. -Y., Lee, Y. W., Kim, H. -S., & Lee, E. -H. (2019). The mediating and moderating effects of meaning in life on the relationship between depression and quality of life in patients with dysphagia. Journal of Clinical Nursing, 28(15–16), 2782–2789. https://doi.org/10.1111/jocn.14907. [Google Scholar] [PubMed] [CrossRef]
Lazarus, R. S., & Folkman, S. (1986). Cognitive theories of stress and the issue of circularity. In: M. H. Appley, R. Trumbull (Eds.), Dynamics of stress (pp. 63–80), Berlin/Heidelberg, Germany: Springer. https://doi.org/10.1007/978-1-4684-5122-1_4 [Google Scholar] [CrossRef]
Liu, J. J. W., Ein, N., Gervasio, J., Battaion, M., Reed, M. et al. (2020). Comprehensive meta-analysis of resilience interventions. Clinical Psychology Review, 82, 101919. https://doi.org/10.1016/j.cpr.2020.101919. [Google Scholar] [PubMed] [CrossRef]
Loseby, P., Schache, K., Cavadino, A., Young, S., Hofman, P. L. et al. (2022). The role of protective psychological factors, self-care behaviors, and HbA1c in young adults with type 1 diabetes. Pediatric Diabetes, 23(3), 380–389. https://doi.org/10.1111/pedi.13306. [Google Scholar] [PubMed] [CrossRef]
Ma, J., & Xiao, Q. (2024). Relationship between self-compassion and compassion for others: The mediated effect of perceived social support and psychological resilience. Psychological Reports, 129, 307–326. https://doi.org/10.1177/00332941241226906. [Google Scholar] [PubMed] [CrossRef]
Menard, S. (1995). Applied logistic regression analysis. Thousand Oaks, CA, USA: Sage. [Google Scholar]
Misurya, I., Misurya, P., & Dutta, A. (2020). The effect of self-compassion on psychosocial and clinical outcomes in patients with medical conditions: A systematic review. Cureus Journal of Medical Science, 12(10), e10998. https://doi.org/10.7759/cureus.10998. [Google Scholar] [PubMed] [CrossRef]
Neff, K. D. (2003). The development and validation of a scale to measure self-compassion. Self and Identity, 2(3), 223–250. https://doi.org/10.1080/15298860390209035 [Google Scholar] [CrossRef]
Neff, K. D., & Dahm, K. A. (2015). Self-compassion: What it is, what it does, and how it relates to mindfulness. In: B. D. Ostafin, M. D. Robinson, B. P. Meier (Eds.), Handbook of mindfulness and self-regulation (pp. 121–137), Berlin/Heidelberg, Germany: Springer. https://doi.org/10.1007/978-1-4939-2263-5_10 [Google Scholar] [CrossRef]
Neff, K. D., & Germer, C. K. (2018). The mindful self-compassion workbook. New York, NY, USA: The Guildford Press. [Google Scholar]
Nie, S., Peng, H., Ju, Q., Liang, Q., Zhang, C. et al. (2023). The relationship between meaning in life and health behaviors in adults aged 55 years and over during the COVID-19 pandemic: The mediating role of risk perception and the moderating role of powerful others health locus of control. International Journal of Behavioral Medicine, 30(3), 388–397. https://doi.org/10.1007/s12529-022-10100-x. [Google Scholar] [PubMed] [CrossRef]
Parviniannasab, A. M., Faramarzian, Z., Hosseini, S. A., Hamidizadeh, S., Bijani, M. et al. (2024). The effect of social support, diabetes management self-efficacy, and diabetes distress on resilience among patients with type 2 diabetes: A moderated mediation analysis. BMC Public Health, 24(1), 477. https://doi.org/10.1186/s12889-024-18022-x. [Google Scholar] [PubMed] [CrossRef]
Pérez-Aranda, A., García-Campayo, J., Gude, F., Luciano, J. V., & Feliu-Soler, A. (2021). Impact of mindfulness and self-compassion on anxiety and depression: The mediating role of resilience. International Journal of Clinical and Health Psychology, 21(2), 21–22. https://doi.org/10.1016/j.ijchp.2021.100229. [Google Scholar] [PubMed] [CrossRef]
Qiu, C., Shao, D., Yao, Y., Zhao, Y., & Zang, X. (2019). Self-management and psychological resilience moderate the relationships between symptoms and health-related quality of life among patients with hypertension in China. Quality of Life Research, 28(9), 2585–2595. https://doi.org/10.1007/s11136-019-02191-z. [Google Scholar] [PubMed] [CrossRef]
Raes, F., Pommier, E., Neff, K. D., & Van Gucht, D. (2011). Construction and factorial validation of a short form of the self-compassion scale. Clinical Psychology & Psychotherapy, 18(3), 250–255. https://doi.org/10.1002/cpp.702. [Google Scholar] [PubMed] [CrossRef]
Sandham, C., & Deacon, E. (2023). The role of self-compassion in diabetes management: A rapid review. Frontiers in Psychology, 14, 1854. https://doi.org/10.3389/fpsyg.2023.1123157. [Google Scholar] [PubMed] [CrossRef]
Schmitt, A., Gahr, A., Hermanns, N., Kulzer, B., Huber, J.et al. (2013). The diabetes self-management questionnaire (DSMQ): Development and evaluation of an instrument to assess diabetes self-care activities associated with glycaemic control. Health and Quality of Life Outcomes, 11(1), 138. https://doi.org/10.1186/1477-7525-11-138. [Google Scholar] [PubMed] [CrossRef]
Shabani, J., & Mahmoudi Tabar, R. (2021). The effectiveness of logotherapy training on psychological well-being and life expectancy in patients with diabetes type 2. Iranian Journal of Diabetes and Obesity, 13(4), 202–207. https://doi.org/10.18502/ijdo.v13i4.7997 [Google Scholar] [CrossRef]
Singer, M. E., Dorrance, K. A., Oxenreiter, M. M., Yan, K. R., & Close, K. L. (2022). The type 2 diabetes ‘modern preventable pandemic’ and replicable lessons from the COVID-19 crisis. Preventive Medicine Reports, 25(7), 101636. https://doi.org/10.1016/j.pmedr.2021.101636. [Google Scholar] [PubMed] [CrossRef]
Skinner, C. M., & Kuijer, R. G. (2024). Self-compassion and health-related quality of life in individuals with endometriosis. Psychology & Health, 40(9), 1479–1496. https://doi.org/10.1080/08870446.2024.2325506. [Google Scholar] [PubMed] [CrossRef]
Steger, M., Frazier, P., Oishi, S., & Kaler, M. (2006). The meaning in life questionnaire: Assessing the presence of and search for meaning in life. Journal of Counseling Psychology, 53(1), 80–93. https://doi.org/10.1037/0022-0167.53.1.80 [Google Scholar] [CrossRef]
Sun, H., Saeedi, P., Karuranga, S., Pinkepank, M., Ogurtsova, K. et al. (2022). IDF diabetes atlas: Global, regional and country-level diabetes prevalence estimates for 2021 and projections for 2045. Diabetes Research and Clinical Practice, 183, 109119. https://doi.org/10.1016/j.diabres.2021.109119. [Google Scholar] [PubMed] [CrossRef]
Tietjen, A. K., Ghandour, R., Mikki, N., Jerden, L., Eriksson, J. W. et al. (2021). Quality of life of type 2 diabetes mellitus patients in Ramallah and al-Bireh Governorate-Palestine: A part of the Palestinian diabetes complications and control study (PDCCS). Quality of Life Research, 30(5), 1407–1416. https://doi.org/10.1007/s11136-020-02733-w. [Google Scholar] [PubMed] [CrossRef]
Trikkalinou, A., Papazafiropou, A. K., Rallatou, M., Kamaratos, A. E., Melidonis, A. et al. (2020). Type 2 diabetes and quality of life. Scientific Chronicles, 25(1), 54–71. https://doi.org/10.4239/wjd.v8.i4.120. [Google Scholar] [PubMed] [CrossRef]
Ueno, Y., & Amemiya, R. (2024). Mediating effects of resilience between mindfulness, self-compassion, and psychological distress in a longitudinal study. Journal of Rational-Emotive & Cognitive-Behavior Therapy, 42(4), 896–906. https://doi.org/10.1007/s10942-024-00553-2 [Google Scholar] [CrossRef]
Visagie, E., Deacon, E., & Kok, R. (2023). Exploring the role of CBT in the self-management of type 2 diabetes: A rapid review. Health SA Gesondheid, 28(1), 1–14. https://doi.org/10.4102/hsag.v28i0.2254. [Google Scholar] [PubMed] [CrossRef]
Wagnild, G., & Young, H. (1993). Development and psychometric evaluation of the resilience scale. Journal of Nursing Measurement, 1(2), 165–178. [Google Scholar] [PubMed]
Wang, R. -H., Chen, S. -Y., Lee, C. -M., Lu, C. -H., & Hsu, H. -C. (2023). Resilience, self-efficacy and diabetes distress on self-management behaviours in patients newly diagnosed with type 2 diabetes: A moderated mediation analysis. Journal of Advanced Nursing, 79(1), 215–222. https://doi.org/10.1111/jan.15483. [Google Scholar] [PubMed] [CrossRef]
Wilson, A. L., McNaughton, D., Meyer, S. B., & Ward, P. R. (2017). Understanding the links between resilience and type-2 diabetes self-management: A qualitative study in South Australia. Archives of Public Health, 75, 56. https://doi.org/10.1186/s13690-017-0222-8. [Google Scholar] [PubMed] [CrossRef]
Wong, C. C. Y., & Yeung, N. C. Y. (2017). Self-compassion and posttraumatic growth: Cognitive processes as mediators. Mindfulness, 8(4), 1078–1087. https://doi.org/10.1007/s12671-017-0683-4 [Google Scholar] [CrossRef]
Wu, D., Ye, B., Tang, C., Xue, J., Yang, Q. et al. (2022). Self-compassion and authentic-durable happiness during COVID-19 pandemic: The mediating role of meaning of life and the moderating role of COVID-19 burnout. Psychology Research and Behavior Management, 15, 3243–3255. https://doi.org/10.2147/PRBM.S380874. [Google Scholar] [PubMed] [CrossRef]
Zipagan, F. B., & Galvez Tan, L. J. T. (2023). From self-compassion to life satisfaction: Examining the mediating effects of self-acceptance and meaning in life. Mindfulness, 14(9), 2145–2154. https://doi.org/10.1007/s12671-023-02183-8 [Google Scholar] [CrossRef]
Cite This Article
 Copyright © 2026 The Author(s). Published by Tech Science Press.
Copyright © 2026 The Author(s). Published by Tech Science Press.This work is licensed under a Creative Commons Attribution 4.0 International License , which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.


 Submit a Paper
Submit a Paper Propose a Special lssue
Propose a Special lssue View Full Text
View Full Text Download PDF
Download PDF Downloads
Downloads
 Citation Tools
Citation Tools